Quick Summary: AI will not replace pathologists but will serve as a collaborative partner that enhances diagnostic accuracy, speed, and efficiency. The technology acts as an augmentation tool, handling repetitive tasks while pathologists focus on complex decision-making, patient care, and contextual interpretation that requires human expertise and clinical judgment.
The question isn’t new. Every medical specialty has faced it as artificial intelligence capabilities expanded. But here’s the thing—pathology represents a unique case where the answer becomes clearer when you understand what pathologists actually do versus what AI can accomplish.
Over 150 years, pathology has transformed remarkably. From humble microscopic tissue examination to today’s revolutionary advancements in digital pathology and AI applications, the field continues evolving. And that evolution tells us something important about the future.
Laboratory test outcomes significantly influence approximately 70% of decisions related to diagnosis, treatment, and patient discharge. That’s a staggering responsibility. So when we ask if AI will replace the professionals behind those decisions, we’re really asking: can algorithms handle the complexity, nuance, and contextual judgment that pathology demands?
The Current State of AI in Pathology
Real talk: AI has already entered pathology labs. It’s not coming—it’s here.
Recent regulatory approvals underscore the practical readiness of this technology. Paige Prostate Detect became the first FDA-cleared AI pathology tool designed specifically for diagnostic assistance. That’s a milestone worth noting because FDA clearance means the technology met rigorous standards for safety and effectiveness.
But FDA approval doesn’t mean replacement. It means augmentation.
According to research published in Diagnostics, AI-assisted diagnosis positions pathologists as partners rather than bystanders. The technology handles specific, well-defined tasks while human expertise manages the broader diagnostic picture.
What AI Actually Does in Pathology
Understanding the replacement question requires clarity about AI’s actual functions. The technology excels at specific, repeatable tasks.
AI systems can scan thousands of tissue slides rapidly, identifying patterns that might take human eyes hours to process. They’re particularly effective at quantitative analysis—counting cells, measuring tissue areas, detecting specific markers with mathematical precision.
Traditional screening for acid-fast positive bacilli in tuberculosis diagnosis is time-consuming and prone to human error due to staining artifacts. AI addresses this by automating detection, reducing workload while maintaining accuracy.
But wait. That’s not replacement—that’s efficiency enhancement.
The College of American Pathologists has explored the transformative role of AI within pathology, noting that these tools provide valuable support for diagnostic workflows. They don’t make final diagnostic decisions independently.
Tasks AI Handles Well
- High-volume initial screening for abnormalities
- Quantitative measurements and cell counting
- Pattern recognition in standardized contexts
- Flagging cases requiring urgent attention
- Consistency checks across large datasets
Where AI Falls Short
Artificial intelligence struggles with contextual interpretation. A pathologist doesn’t just look at tissue under a microscope—they integrate clinical history, lab results, imaging findings, and patient-specific factors.
Consider a biopsy showing atypical cells. Is it early cancer? A reactive process? An artifact from sample preparation? The answer often depends on clinical context AI doesn’t possess.
According to research on AI in laboratory medicine, while AI shows promise in diagnostics and patient management, significant challenges remain regarding implementation, particularly in complex decision-making scenarios.

Integrating AI Into Business Systems With AI Superior
AI Superior works with companies that need AI to operate as part of existing systems. The focus is on connecting models to real workflows and ensuring they deliver consistent results in practice.
Looking to Connect AI With Your Current Systems?
AI Superior can help with:
- developing AI components for specific use cases
- evaluating use cases and technical direction
- integrating AI into existing infrastructure
👉 Contact AI Superior to discuss your project, data, and implementation approach
The Partnership Model: How Pathologists and AI Collaborate
Here’s where it gets interesting. The most successful AI implementations don’t replace pathologists—they amplify their capabilities.
Think of AI as a highly specialized assistant that never gets tired, works at incredible speed, but needs supervision and contextual guidance. Pathologists provide that guidance while AI handles the computational heavy lifting.
Research on reducing medical diagnosis workload through AI emphasizes that the technology addresses challenges such as increasing diagnostic demands and staff burnout. It doesn’t eliminate the need for medical professionals—it makes their work more sustainable.
| Diagnostic Phase | AI Role | Pathologist Role |
|---|---|---|
| Initial Screening | Rapid scan, flag abnormalities | Review flagged cases, set priorities |
| Quantitative Analysis | Precise measurements, cell counts | Interpret significance, clinical relevance |
| Pattern Recognition | Identify known patterns at scale | Recognize unusual variants, exceptions |
| Final Diagnosis | Provide data support | Make diagnostic decision, clinical integration |
| Reporting | Generate standardized elements | Contextualize findings, recommendations |
The Pathology Precision Network, mentioned in College of American Pathologists resources, brings together industry, academia, and clinical pathology to advance AI integration. Members get early access to AI-powered tools and participate in evidence generation. That’s collaboration, not replacement.
Why Complete Replacement Isn’t Realistic
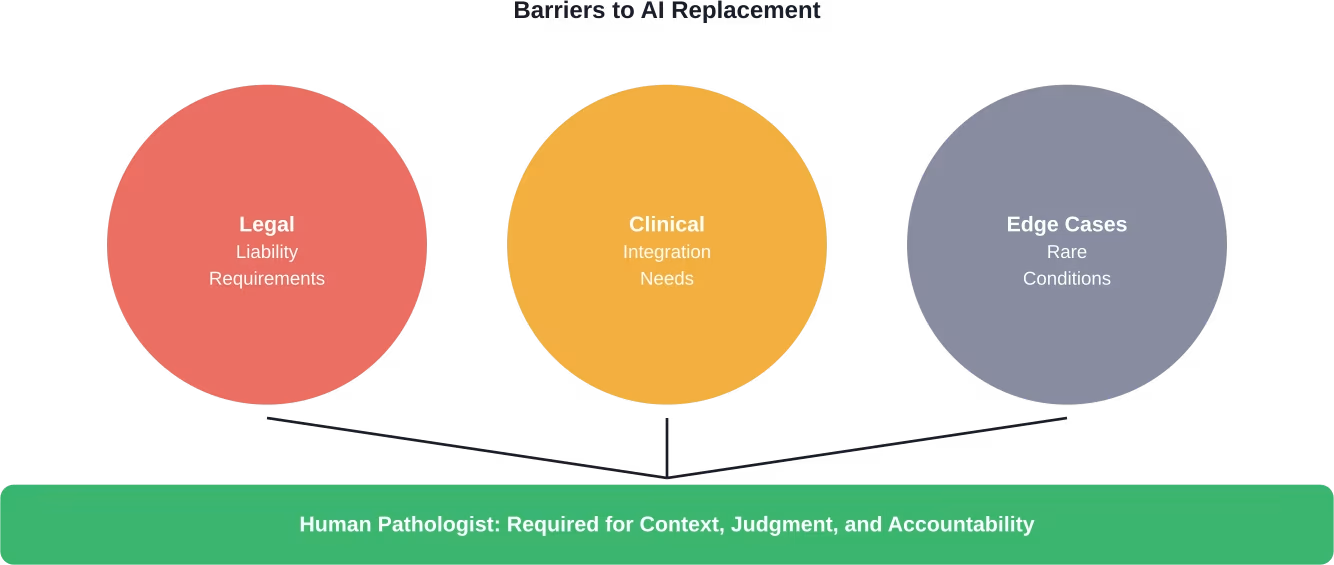
Several fundamental barriers prevent AI from replacing pathologists entirely.
First, regulatory and legal frameworks. Diagnostic responsibility carries legal implications. Who’s liable when an AI makes an error? Current medical malpractice frameworks require a licensed physician to take diagnostic responsibility. That’s not changing anytime soon.
Second, the clinical integration challenge. Pathology doesn’t exist in isolation. Pathologists regularly consult with surgeons, oncologists, and other specialists. They participate in tumor boards, discuss treatment options, and provide nuanced guidance that extends far beyond slide reading.
Third, edge cases and rare conditions. AI models train on available data. Rare diseases, unusual presentations, and novel conditions require human expertise, medical literature knowledge, and sometimes consultation networks that AI can’t replicate.
The Impact on Pathology Careers and Workload
So what does AI actually mean for pathology professionals? The answer is more nuanced than simple job preservation.
Research on AI’s role in addressing burnout and healthcare workforce dynamics shows that AI has immense potential to reduce workload pressures. Burnout has become ubiquitous among physicians and staff workers, markedly impairing healthcare workforce sustainability.
AI doesn’t eliminate pathologist positions—it transforms them. Routine screening tasks become automated, freeing pathologists to focus on complex cases, consultation, education, and research.
Various stakeholders express mixed perspectives on AI integration. Some pathologists express concern about workflow changes and learning curves. Others see AI as a solution to increasing case volumes and workforce shortages.
The shift mirrors what happened with digital pathology adoption. Initial resistance gave way to recognition that digital tools enhanced rather than threatened the profession.
Skills That Become More Valuable
- Clinical correlation and context integration
- Complex case interpretation and consultation
- AI tool oversight and quality assurance
- Multidisciplinary team collaboration
- Novel pathology research and discovery
What the Future Actually Holds
Predictions about AI in pathology need grounding in current trajectories rather than speculation.
Digital pathology infrastructure continues expanding. More labs adopt whole-slide imaging, creating the foundation AI tools require. But adoption rates vary significantly across institutions and regions.
Regulatory frameworks are developing. FDA approvals like Paige Prostate Detect establish precedents for AI diagnostic tools. Future regulations will likely focus on validation standards, performance monitoring, and integration protocols.
Research published on pathology in the artificial intelligence era emphasizes that AI serves as a tool for augmentation rather than replacement. The integration preserves human insight while leveraging computational capabilities.
Training programs are evolving. Pathology residencies increasingly include digital pathology and AI fundamentals. Tomorrow’s pathologists will view AI as a standard tool, much like today’s pathologists view immunohistochemistry.
Practical Implementation Challenges
Theory and practice diverge when implementing AI in real clinical settings.
Cost represents a significant barrier. AI systems require substantial investment in hardware, software, training, and maintenance. Smaller practices and facilities in lower-resource settings face accessibility challenges.
Research on AI advancement in laboratory medicine in low- and middle-income countries highlights that while AI promises healthcare improvements, implementation challenges include increasing costs and resource constraints.
Data quality matters enormously. AI models perform only as well as their training data. Variability in staining protocols, scanning equipment, and sample preparation creates consistency challenges.
Workflow integration requires careful planning. Adding AI tools without disrupting established diagnostic processes demands thoughtful implementation strategies and staff training.
| Challenge | Impact Level | Mitigation Strategy |
|---|---|---|
| Initial Investment Cost | High | Phased implementation, shared resources |
| Staff Training Requirements | Medium | Structured education programs, vendor support |
| Data Standardization | High | Protocol harmonization, quality controls |
| Regulatory Compliance | Medium | Professional society guidance, validation studies |
| Workflow Disruption | Medium | Pilot programs, iterative refinement |
Frequently Asked Questions
Will pathologists lose their jobs to AI?
No. AI serves as an augmentation tool rather than a replacement. Pathologists remain essential for diagnostic decision-making, clinical context integration, and patient care coordination. The technology handles specific tasks while human expertise manages the broader diagnostic picture and assumes legal responsibility.
How accurate is AI compared to human pathologists?
AI accuracy varies by task and context. For well-defined, repetitive tasks like cell counting or standardized pattern recognition, AI can match or exceed human performance. However, overall diagnostic accuracy requires contextual judgment and clinical integration where human pathologists remain superior. The best outcomes come from human-AI collaboration.
What tasks will AI handle in pathology?
AI excels at high-volume screening, quantitative analysis, pattern recognition in standardized contexts, and flagging cases requiring urgent attention. It handles computational tasks efficiently while pathologists focus on interpretation, clinical correlation, complex decision-making, and patient communication.
Do pathologists need to learn AI programming?
Not necessarily. Understanding AI principles, capabilities, and limitations matters more than programming skills. Pathologists need to know how to validate AI outputs, recognize when results require human review, and integrate AI insights into diagnostic workflows. Technical AI development typically involves separate specialists.
How long before AI becomes standard in pathology labs?
AI adoption is already underway but varies significantly across institutions. FDA-approved tools like Paige Prostate Detect demonstrate regulatory acceptance. Full integration depends on infrastructure development, cost reduction, regulatory evolution, and workflow optimization—likely a gradual process over the next decade rather than a sudden shift.
Will AI improve diagnostic accuracy?
AI has the potential to reduce diagnostic errors by providing second-opinion support, catching overlooked findings, and maintaining consistency across high case volumes. However, accuracy improvements depend on proper implementation, adequate training data, appropriate clinical context, and effective pathologist oversight.
What happens to pathology training programs?
Training programs are evolving to include digital pathology fundamentals and AI literacy. Future pathologists will learn to work alongside AI tools as standard practice. Emphasis shifts toward skills AI can’t replicate—clinical reasoning, complex interpretation, consultation, and integrative thinking—while incorporating AI competencies.
Conclusion
The answer to whether AI will replace pathologists is definitively no. But that doesn’t mean pathology remains unchanged.
AI transforms pathology through augmentation—enhancing speed, accuracy, and efficiency while pathologists retain diagnostic authority and clinical judgment. The technology handles computational tasks that machines do best, freeing human expertise for what requires contextual understanding, integration, and professional judgment.
Successful pathology practices will embrace AI as a collaborative partner. Those who resist technological integration risk falling behind, while those who thoughtfully incorporate AI tools position themselves for sustainable, effective practice.
The future of pathology isn’t human versus machine. It’s human and machine, working together to deliver better patient care, more accurate diagnoses, and more sustainable medical practice. That collaboration has already begun.
