Key Points: Implementing artificial intelligence in healthcare involves multiple cost components including software licensing ($50,000-$500,000+), infrastructure investment (hardware, cloud services), data preparation, staff training, and ongoing maintenance. Recent systematic reviews show AI interventions can achieve cost-effectiveness with incremental cost-effectiveness ratios below accepted thresholds, particularly in oncology, cardiology, and ophthalmology, though comprehensive economic evaluations remain limited.
Healthcare organizations face mounting pressure to control costs while improving patient outcomes. AI promises to deliver both—but the path from promise to implementation requires serious financial commitment.
The economics of artificial intelligence in healthcare remain complex. While some AI interventions demonstrate clear cost savings, others require substantial upfront investment with uncertain returns. Understanding these costs matters for anyone responsible for healthcare technology decisions.
This guide breaks down the actual costs of implementing AI in healthcare settings, drawing from systematic reviews, economic evaluations, and real-world deployment data. No hype. Just the numbers and factors that shape healthcare AI budgets in 2026.
The Economic Reality of Healthcare AI
Recent systematic reviews paint a nuanced picture of AI’s economic impact across healthcare settings. A comprehensive analysis published in NPJ Digital Medicine examined cost-effectiveness and budget impact studies across multiple clinical domains. The findings? Mixed, but increasingly promising.
Nineteen studies spanning oncology, cardiology, ophthalmology, and infectious diseases demonstrate that AI improves diagnostic accuracy, enhances quality-adjusted life years, and reduces costs—largely by minimizing unnecessary procedures and optimizing resource use. Several interventions achieved incremental cost-effectiveness ratios well below accepted thresholds.
But here’s the catch.
Many evaluations relied on static models that may overestimate benefits by not capturing the adaptive learning of AI systems over time. Indirect costs, infrastructure investments, and equity considerations were often underreported, suggesting that reported economic benefits may be overstated.
Healthcare costs keep rising. PwC’s Health Research Institute projected healthcare expenses to increase by 8% in 2025 (per ITRex source material). Technologies like AI can potentially break this cycle—but only when organizations understand the full cost picture.
Breaking Down AI Implementation Costs
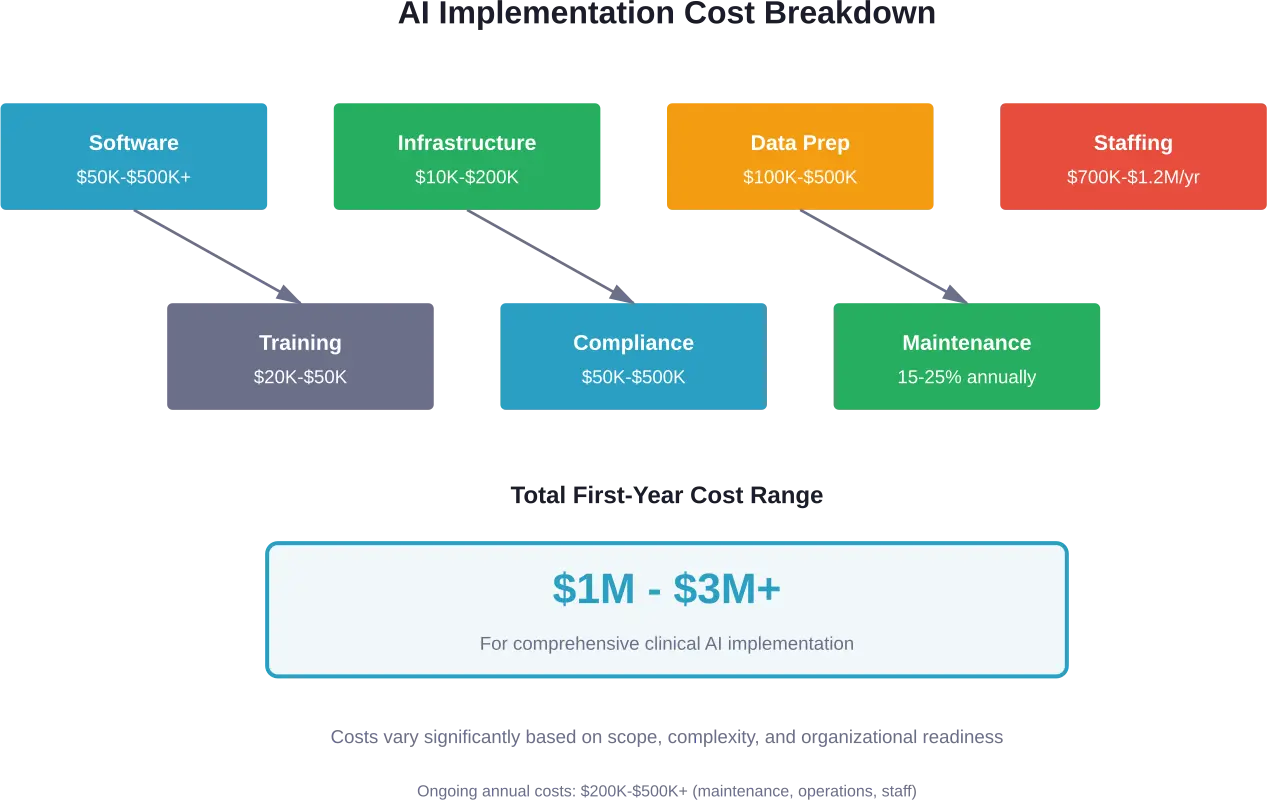
The cost of implementing AI in healthcare splits into several major categories. Each organization will weight these differently based on their specific use case, existing infrastructure, and strategic goals.
Software Licensing and Development
Commercial AI software for healthcare comes with significant licensing fees. The range varies dramatically based on capability, scale, and vendor.
According to economic evaluation data from the HosmartAI Horizon 2020 Project, each technical solution was developed with dedicated funding of 50,000 EUR. This represents the lower end for custom development of specialized clinical AI tools.
For enterprise-grade AI systems, costs escalate rapidly. Healthcare organizations typically face annual licensing fees that vary significantly depending on the number of users, data volume, and feature complexity, with commercial solutions ranging broadly in cost.
Custom development costs even more. Building a proprietary AI system requires data scientists, machine learning engineers, and domain experts working for months or years. Total development costs frequently exceed $1 million for sophisticated clinical AI applications.
Infrastructure and Hardware
AI systems demand substantial computational resources. Organizations must choose between on-premises infrastructure, cloud services, or edge AI deployments—each with different cost profiles.
| Deployment Method | Upfront Cost | Ongoing Cost | Best For
|
|---|---|---|---|
| On-Premises | High (hardware purchase) | Medium (maintenance, power) | Organizations with data sovereignty requirements |
| Cloud-Based | Low (no hardware) | Variable (usage-based) | Scalable deployments, faster time-to-value |
| Edge AI | Medium (edge devices) | Low (minimal cloud costs) | Real-time processing, low-latency applications |
Cloud infrastructure costs scale with usage. Organizations running intensive AI workloads can spend $10,000 to $100,000+ monthly on cloud computing resources, storage, and data transfer.
On-premises deployments require purchasing high-performance GPU servers. A single enterprise-grade server with multiple GPUs suitable for AI training runs $50,000 to $200,000, plus ongoing power and cooling costs.
Data Preparation and Management
Data is the foundation of any AI system. But raw healthcare data rarely arrives ready for AI consumption.
Data preparation typically consumes 60-80% of AI project timelines. This includes data cleaning, normalization, annotation, and integration from disparate systems. For a mid-sized healthcare organization, data preparation costs easily reach $100,000 to $500,000 for a single AI initiative.
Medical data annotation requires clinical expertise, with specialists labeling training data at various rates depending on specialization and experience. Annotating thousands of medical images or records for a single AI model can cost $50,000 to $200,000 alone.
Ongoing data management adds recurring costs for storage, security, backup, and compliance monitoring. Healthcare data storage involves recurring costs that vary based on performance requirements and redundancy levels.
Staffing and Expertise
Implementing and maintaining AI systems requires specialized talent—and talent comes expensive.
According to job market data from Glassdoor and Dice, key roles command substantial salaries. An AI director who might lead the AI group averages about $200,000 in total compensation. Project managers focused on AI initiatives average $121,110. Data scientists earn approximately $106,130 on average.
These figures represent averages. In competitive markets or for senior positions, salaries escalate significantly. A team of 5-7 specialists supporting healthcare AI initiatives can easily cost $700,000 to $1.2 million annually in salaries alone, before benefits and overhead.
Many organizations lack this expertise internally. They turn to consultants or implementation partners, which may charge varying rates for specialized AI consulting in healthcare contexts.
Training and Change Management
Technology alone doesn’t deliver value. Clinical staff must understand how to use AI tools effectively and trust the recommendations they provide.
Training programs for clinical AI tools vary in scope and cost. Comprehensive training programs typically cost $20,000-$50,000 or more including curriculum development, trainer time, and materials. Larger deployments across multiple departments or facilities scale proportionally.
Change management represents a hidden cost many organizations underestimate. Resistance to AI adoption, workflow disruption, and integration challenges can impact value realization. Organizations investing in formal change management generally see better outcomes.
Compliance and Security
Healthcare AI must meet stringent regulatory requirements. HIPAA compliance, FDA approvals for clinical decision support tools, and emerging AI-specific regulations create significant cost obligations.
Security infrastructure for AI systems includes encryption, access controls, audit logging, and continuous monitoring. Initial security implementation for a healthcare AI system typically costs $50,000-$150,000, with ongoing security operations adding $30,000-$100,000 annually.
Regulatory compliance consulting for AI medical devices or clinical tools runs $100,000-$500,000+ depending on the pathway and complexity. Organizations developing novel clinical AI applications face the highest regulatory costs.
Maintenance and Updates
AI systems require ongoing maintenance. Models degrade over time as data distributions shift. Security patches, performance optimization, and feature enhancements demand continuous investment.
Ongoing maintenance represents a significant recurring expense, typically estimated as a percentage of initial implementation costs. For a $500,000 AI implementation, expect substantial annual maintenance expenses.
Model retraining represents a significant ongoing cost. Clinical AI models often require quarterly or annual retraining to maintain performance. Each retraining cycle consumes compute resources and data science time—budget $10,000-$50,000 per retraining event for complex clinical models.

Assess Healthcare AI Costs with Domain-Specific Expertise from AI Superior
AI in healthcare involves additional cost drivers such as regulatory compliance, data security, validation standards, and integration with clinical systems. AI Superior supports healthcare organizations with technically sound and compliant AI planning.
They help with:
- Data privacy and regulatory considerations
- Model validation and performance evaluation
- Integration with existing healthcare systems
- Risk mitigation strategies
If you are budgeting for AI in healthcare, consult AI Superior for a detailed cost assessment aligned with both technical and regulatory requirements.
Cost-Effectiveness Evidence from Clinical Domains
How does AI actually perform economically across different healthcare specialties? Recent systematic reviews provide concrete evidence.
Oncology Applications
AI interventions in oncology show promising cost-effectiveness, particularly in early detection and treatment planning. One study showed a 17.6% boost in breast cancer detection with AI-assisted mammography compared to standard screening.
Improved early detection translates to reduced treatment costs. Cancers caught earlier require less aggressive—and less expensive—interventions. Economic models suggest AI-enhanced screening programs can achieve incremental cost-effectiveness ratios well below accepted thresholds of $50,000-$100,000 per quality-adjusted life year.
But context matters. Cost-effectiveness depends heavily on population risk profiles, screening intervals, and local healthcare costs. AI screening tools that perform well economically in high-risk populations may not justify costs in average-risk settings.
Cardiology and Diagnostic Imaging
Cardiac imaging AI demonstrates strong economic value by reducing interpretation time and improving diagnostic accuracy. AI systems can detect subtle abnormalities in echocardiograms, cardiac MRI, and CT angiography that human readers might miss.
The economic benefit comes from two sources: catching problems earlier when they’re cheaper to treat, and reducing false positives that lead to unnecessary downstream testing.
Economic evaluations from the HosmartAI project examined AI diagnostic systems in cardiology settings. The interventions improved diagnostic accuracy while reducing unnecessary specialized examinations—a key driver of cost savings.
Ophthalmology and Diabetic Retinopathy
AI screening for diabetic retinopathy represents one of healthcare AI’s clearest economic wins. Automated screening reduces the need for specialist ophthalmologist reviews while maintaining high diagnostic accuracy.
The cost structure favors AI here. Traditional screening requires expensive specialist time. AI systems can screen patients at primary care visits, catching problems earlier and reducing vision loss—which carries enormous quality-of-life and economic costs.
Multiple economic evaluations show diabetic retinopathy AI screening achieving cost-effectiveness ratios well below standard thresholds, particularly in underserved populations with limited access to ophthalmologists.
Clinical Documentation and Administrative Tasks
Large language models are transforming clinical documentation. These AI systems can listen during patient visits and draft clinical notes automatically, cutting documentation time by more than 60% according to recent studies.
The economic impact is substantial. Clinicians spend 30-50% of their time on documentation. Reducing this burden allows seeing more patients or spending more time in direct patient care—both valuable outcomes.
Documentation AI typically costs $100-$300 per clinician monthly. For a physician generating $500,000+ in annual revenue, even small time savings justify the cost many times over.
Factors That Drive AI Costs Higher or Lower
Not all AI implementations cost the same. Several factors significantly influence total costs.
System Complexity and Customization
Off-the-shelf AI solutions cost less than custom development. A commercial AI tool for a well-defined use case might cost $50,000-$200,000 annually. Custom AI development for novel clinical applications easily exceeds $1 million.
Model complexity matters too. Simple rule-based systems or traditional machine learning models cost less to develop and maintain than deep learning systems requiring massive datasets and computational resources.
Integration Requirements
AI systems must integrate with electronic health records, imaging systems, laboratory systems, and other healthcare IT infrastructure. Integration complexity drives significant cost variation.
Simple integrations using standard APIs might cost $20,000-$50,000. Complex integrations requiring custom middleware, data transformation, and workflow redesign can cost $200,000-$500,000.
Legacy systems make integration harder and more expensive. Organizations running older EHR systems face higher integration costs than those on modern, API-enabled platforms.
Data Volume and Quality
More data doesn’t always mean better AI—but it usually means higher costs. Large datasets require more storage, more compute for training, and more time for data scientists to process and validate.
Poor data quality multiplies costs. If existing healthcare data lacks standardization, contains errors, or sits in incompatible formats, data cleanup becomes the project’s dominant expense.
Organizations with mature data governance and high-quality structured data implement AI faster and cheaper than those starting from messy, unstructured data environments.
Regulatory Pathway
AI systems that qualify as medical devices face FDA oversight and significantly higher regulatory costs. The regulatory pathway depends on the AI’s intended use and risk classification.
Clinical decision support tools that inform rather than direct clinical decisions may qualify for exemptions. AI that directly diagnoses or recommends treatments typically requires formal FDA clearance or approval—adding $100,000-$500,000+ in regulatory costs.
Post-market surveillance and ongoing regulatory compliance add recurring costs for regulated AI medical devices.
Organizational Readiness
Organizations with existing data science capabilities, modern IT infrastructure, and AI-literate staff implement new AI initiatives faster and cheaper.
Those starting from scratch must build foundational capabilities first. Establishing data infrastructure, hiring talent, and developing organizational AI literacy can cost $500,000-$2 million before deploying the first production AI system.

Government and CMS Perspectives on AI Costs
The Centers for Medicare & Medicaid Services is actively exploring technology-enabled care and AI to improve outcomes while controlling costs. CMS initiatives provide insight into how payers view AI economics.
The WISeR Model
The Wasteful and Inappropriate Service Reduction Model leverages AI and machine learning to ensure appropriate Medicare payment. This voluntary model uses enhanced technologies along with human clinical review to reduce wasteful spending.
The model encourages care navigation and evidence-supported best practices. By identifying potentially inappropriate services before payment, CMS aims to protect taxpayer dollars while maintaining quality care.
Technology-Enabled Care Initiatives
According to a December 2025 CMS blog post, technology-enabled care and outcome-aligned payments represent key innovation priorities. The CMS Innovation Center is exploring how technology-supported care can improve patient outcomes and make care delivery more effective and efficient.
These initiatives recognize that while technology has transformed daily life, healthcare for many people with Medicare has not kept pace. Millions live with chronic conditions that could benefit from technology-enabled monitoring and intervention.
Medicaid Technology Pledges
In January 2026, several health technology companies pledged to CMS that they would help states implement Medicaid system improvements. One company committed to providing a fraud detection tool at a discounted price of $2 million per state in one-time implementation costs.
This tool identifies individual applications most at risk of being fraudulent based on various data sets. States can add customization and additional services as needed. The pricing illustrates the scale of investment states face for AI-powered administrative improvements.
Hidden Costs and Overlooked Expenses
Total cost of ownership extends beyond obvious line items. Several hidden costs catch organizations unprepared.
Data Governance and Privacy
AI systems amplify data governance requirements. Organizations must establish clear policies for AI data use, patient consent, and privacy protection.
Building comprehensive data governance for AI typically costs $100,000-$300,000 in consulting, policy development, and initial implementation. Ongoing governance operations add $50,000-$150,000 annually.
Model Monitoring and Performance Management
AI models don’t maintain performance automatically. Continuous monitoring detects degradation, bias, and errors. Building monitoring infrastructure and processes costs $50,000-$200,000 initially, plus ongoing operational costs.
When monitoring detects problems, intervention costs follow. Model retraining, adjustment, or replacement can cost $50,000-$300,000 per incident depending on severity.
Vendor Risk and Lock-In
Commercial AI vendors may change pricing, discontinue products, or go out of business. Organizations face risk if they build critical workflows around vendor-dependent AI.
Mitigating vendor risk requires architectural choices that preserve flexibility—typically costing 15-25% more upfront than vendor-locked approaches. But this investment pays off when vendors change terms or disappear.
Opportunity Costs
Resources invested in AI implementation can’t be used elsewhere. Organizations must weigh AI investments against alternative uses of capital and staff time.
A $2 million AI project represents significant opportunity cost—money that could hire clinicians, upgrade facilities, or fund other initiatives. Smart organizations evaluate AI ROI against these alternatives, not just in isolation.
Strategies to Control AI Implementation Costs
Several approaches help organizations implement AI more cost-effectively without sacrificing quality or outcomes.
Start Small and Prove Value
Pilot projects cost less than full-scale deployments. Starting with a single department or use case allows proving value before major investment.
A focused pilot might cost $100,000-$300,000 versus $1-3 million for enterprise deployment. Pilots that demonstrate clear ROI justify larger investments. Those that don’t save organizations from expensive failures.
Leverage Cloud and SaaS Models
Cloud-based AI solutions convert capital expenses to operational expenses. Instead of buying hardware and building infrastructure, organizations pay monthly or annually for what they use.
This approach reduces upfront costs and financial risk. Cloud vendors handle maintenance, updates, and scaling. Organizations avoid being stuck with depreciated hardware if an AI initiative doesn’t work out.
Partner with Academic Medical Centers
Academic partnerships can reduce development costs. Academic medical centers often seek clinical partners for AI research. They may provide technical expertise, data science resources, or even funding in exchange for access to data and clinical validation opportunities.
These partnerships work best when interests align. The academic center gets research opportunities and publications. The healthcare organization gets AI capabilities at reduced cost.
Prioritize Data Quality Early
Investing in data quality upfront saves money later. Clean, well-structured data reduces development time, improves model performance, and decreases ongoing maintenance costs.
Organizations should audit data quality before starting AI initiatives. Fixing data problems costs less before building AI systems that depend on that data.
Build Internal Capabilities Gradually
Hiring a full AI team immediately is expensive. A phased approach starts with one or two key hires plus consulting support, gradually building internal capabilities.
Early hires should focus on AI strategy and vendor management rather than deep technical skills. As the organization matures, add data scientists and engineers. This approach spreads staffing costs over time while building sustainable capabilities.
Measuring ROI and Cost-Effectiveness
How should healthcare organizations evaluate whether AI investments deliver value? Several frameworks help measure AI ROI.
Incremental Cost-Effectiveness Ratios
Health economists use incremental cost-effectiveness ratios to compare interventions. This metric divides the additional cost of an intervention by its additional benefit, typically measured in quality-adjusted life years.
Accepted ICER thresholds vary by country and context. In the United States, interventions with ICERs below $50,000-$100,000 per quality-adjusted life year are generally considered cost-effective. Several AI interventions in the systematic review literature achieved ICERs well below these thresholds.
Budget Impact Analysis
Budget impact differs from cost-effectiveness. Even highly cost-effective interventions may strain budgets if upfront costs are high or if many patients qualify for treatment.
Budget impact analysis examines total financial impact over specific time periods. Organizations should conduct both cost-effectiveness and budget impact analyses—an intervention might be cost-effective long-term but financially infeasible given current budgets.
Time Savings and Productivity Gains
Clinical AI often saves time more than money directly. Documentation AI that saves 30 minutes per clinician daily creates substantial value even if it doesn’t reduce headcount.
Quantifying time savings requires measuring baseline workflows, monitoring AI-enabled workflows, and calculating the economic value of saved time. For highly compensated specialists, even small time savings justify significant AI costs.
Quality Metrics and Outcomes
Some AI benefits resist easy financial quantification. Improved diagnostic accuracy, reduced medical errors, and better patient satisfaction create real value that may not appear directly on financial statements.
Comprehensive ROI calculations should include both financial and quality metrics. A balanced scorecard approach captures multiple dimensions of value creation.
| ROI Metric | What It Measures | Best Used For | Limitations
|
|---|---|---|---|
| ICER | Cost per quality-adjusted life year gained | Clinical interventions with health outcomes | Requires clinical trial data or models |
| Budget Impact | Total financial effect over time period | Evaluating financial feasibility | Doesn’t capture long-term value |
| Time Savings | Clinician hours saved | Documentation, administrative AI | Assumes saved time creates value |
| Error Reduction | Decrease in diagnostic/treatment errors | Decision support, diagnostic AI | Difficult to measure baseline accurately |
| Simple Payback | Time to recover initial investment | Quick feasibility assessment | Ignores time value of money |
Real-World Implementation Timelines and Costs
What do actual AI implementations look like from start to finish? Timelines and costs vary, but typical patterns emerge.
Small-Scale Pilot Implementation
A focused pilot targeting a single clinical use case typically follows this timeline:
Months 1-2: Requirements gathering, vendor selection, contract negotiation. Costs: $20,000-$50,000 in staff time and consulting.
Months 3-4: Data preparation, integration, and testing. Costs: $30,000-$100,000 for data work and integration.
Months 5-6: Pilot deployment, training, and evaluation. Costs: $20,000-$50,000 for training and evaluation.
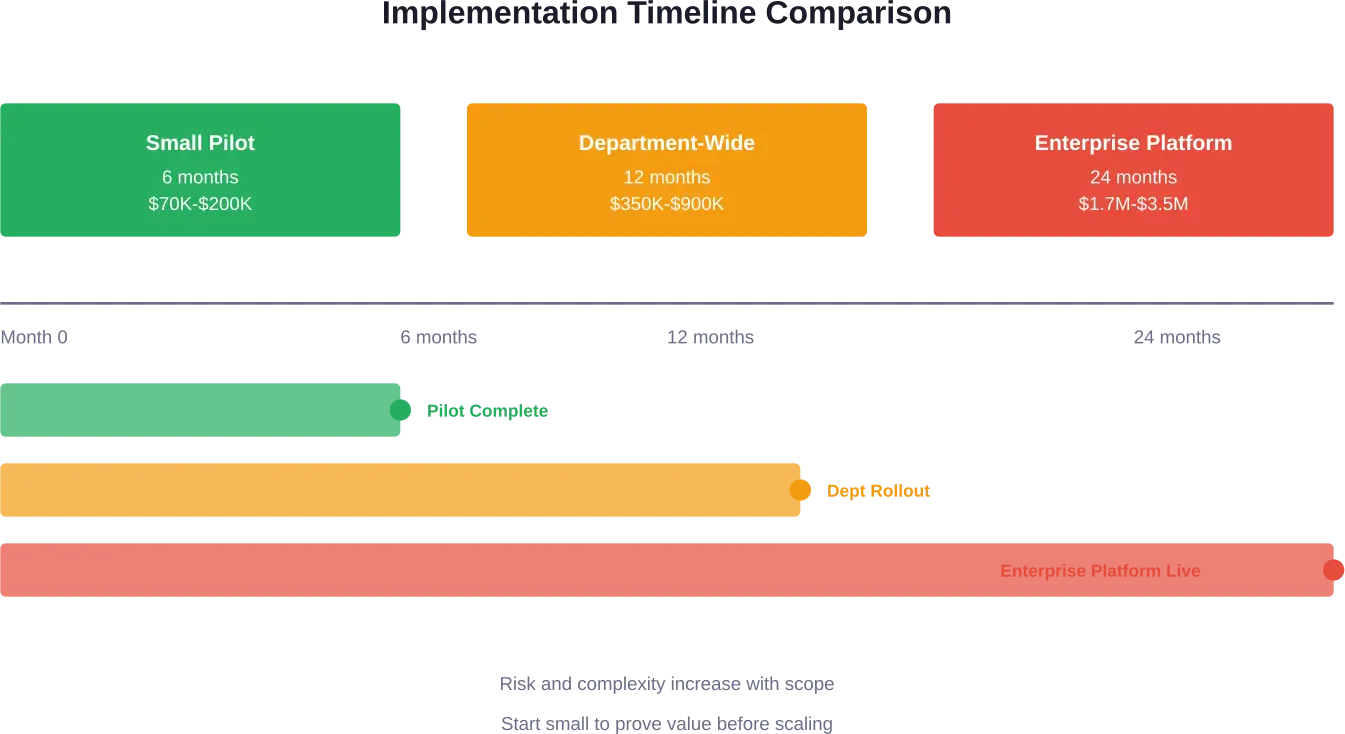
Total timeline: 6 months. Total cost: $70,000-$200,000 plus software licensing fees.
Department-Wide Implementation
Deploying AI across an entire department—radiology, pathology, or cardiology—requires more time and investment:
Months 1-3: Planning, stakeholder alignment, and detailed requirements. Costs: $50,000-$100,000.
Months 4-8: Infrastructure setup, integration development, and testing. Costs: $200,000-$500,000.
Months 9-12: Phased rollout, training, and optimization. Costs: $100,000-$300,000.
Total timeline: 12 months. Total cost: $350,000-$900,000 plus software and infrastructure.
Enterprise AI Platform
Building an enterprise AI platform to support multiple use cases across the organization represents the largest investment:
Months 1-6: Strategy, architecture, and platform selection. Costs: $200,000-$500,000.
Months 7-18: Platform deployment, integration, and initial use cases. Costs: $1-2 million.
Months 19-24: Additional use cases, optimization, and governance. Costs: $500,000-$1 million.
Total timeline: 24 months. Total cost: $1.7-3.5 million plus ongoing operations.
Methodological Limitations in AI Cost Studies
The systematic review literature reveals important gaps in how AI costs are evaluated. Understanding these limitations helps interpret published cost-effectiveness claims.
Static Versus Dynamic Modeling
Most economic evaluations use static models that assume AI performance remains constant over time. In reality, AI systems learn and adapt—potentially improving or degrading based on new data and changing environments.
Static models may overestimate benefits by not capturing performance degradation. They may also underestimate benefits by missing continuous improvement from adaptive learning. Dynamic modeling indicates sustained long-term value, but further research is needed.
Incomplete Cost Accounting
Published studies often underreport infrastructure investments, indirect costs, and equity considerations. This incomplete accounting suggests that reported economic benefits may be overstated.
Comprehensive cost-consequence analyses capture more dimensions. The HosmartAI economic evaluation used a Cost Consequence Analysis approach that examined multiple cost and outcome components separately, providing more nuanced insights than simple cost-effectiveness ratios.
Short Time Horizons
Many studies evaluate AI over relatively short time periods—one to three years. AI investments often require longer periods to achieve full value, especially when accounting for organizational learning and process optimization.
Longer time horizons would capture sustained benefits but also reveal hidden long-term costs like ongoing model maintenance, periodic retraining, and eventual system replacement.
Lack of Subgroup Analyses
AI systems may perform differently across patient subgroups defined by demographics, disease severity, or healthcare setting. Economic evaluations rarely examine these variations.
An AI intervention highly cost-effective for one population may perform poorly for another. Context-specific evaluations would provide better guidance for implementation decisions.
The WHO Perspective on Digital Health Economics
The World Health Organization has been working with health authorities to promote digital tools that enhance data-driven policies and cost-effective use of public funds and human resources.
In the Republic of Moldova, WHO supported the development of digital automation tools for medicine price monitoring and reimbursement decisions. These tools allow automated aggregation of drug prices from European reference countries, helping set maximum prices on the Moldovan market.
According to the Director General of the Medicines and Medical Devices Agency, the automated monitoring optimizes staff time and increases response speed to price registration requests, increasing medicine variety and affordability for patients.
The WHO Universal Health Coverage Adviser noted: “Everyone is talking about AI these days, and certainly this new technology is already changing the face of modern medicine. But scaling up this technology to the level of national health-care systems requires significant time and financial resources that are not quick to mobilize. Until then, there are at disposal efficient digital automation solutions that can increase the value of the time spent on daily tasks by health-care professionals.”
This perspective acknowledges AI’s transformative potential while recognizing that simpler digital automation may offer better near-term value for resource-constrained health systems.
Common Mistakes That Inflate AI Costs
Organizations make predictable mistakes that drive AI costs higher than necessary. Avoiding these pitfalls improves cost-effectiveness.
Overengineering Solutions
The most sophisticated AI isn’t always the best choice. Deep learning models require more data, more compute, and more expertise than simpler approaches.
Many problems yield to traditional machine learning or even rule-based systems at a fraction of the cost. Organizations should match solution complexity to problem complexity—not chase cutting-edge AI for its own sake.
Skipping Data Assessment
Launching AI initiatives without assessing data quality and availability leads to expensive surprises. Organizations discover too late that their data is incomplete, inconsistent, or inaccessible.
A thorough data assessment costs $20,000-$50,000 but saves multiples of that by identifying problems early when they’re cheaper to fix.
Underestimating Change Management
Technical implementation represents only part of the challenge. Clinical adoption requires training, workflow redesign, and addressing resistance.
Organizations that skimp on change management see poor adoption and limited value realization. Investing appropriately in change management significantly improves outcomes.
Vendor Over-Reliance
Vendors have incentives to maximize scope and complexity. Organizations without internal AI expertise struggle to evaluate vendor claims or push back on unnecessary features.
Even a small internal team or trusted advisor can help organizations negotiate better contracts and avoid overpaying for capabilities they don’t need.
Ignoring Total Cost of Ownership
Focusing solely on initial implementation costs misses the bigger picture. Ongoing operations, maintenance, and eventual replacement often exceed initial costs over system lifetimes.
Smart organizations model 5-7 year total cost of ownership before committing to AI initiatives. This longer view reveals different cost structures and sometimes changes vendor or approach decisions.
Future Cost Trends in Healthcare AI
How will AI costs evolve? Several trends suggest where costs are heading.
Decreasing Compute Costs
Cloud computing costs continue declining. GPU performance improves while prices hold steady or drop. These trends make AI more accessible to smaller organizations.
What cost $100,000 in compute resources three years ago might cost $30,000-$50,000 today. This trajectory continues, though perhaps at slower rates as efficiency gains become harder.
Rising Talent Costs
Demand for AI talent outpaces supply. Salaries for data scientists, machine learning engineers, and AI specialists continue climbing.
This trend may reverse as more universities graduate AI-trained professionals, but shortages persist in 2026 and show few signs of easing soon.
Maturing Commercial Solutions
Healthcare AI software is maturing. More vendors offer proven, FDA-cleared solutions for common use cases. Competition drives prices down while quality improves.
Organizations benefit from vendor competition and product maturity. Use cases that required custom development five years ago now have multiple commercial options at lower prices.
Increased Regulatory Costs
Regulatory scrutiny of healthcare AI is intensifying. FDA guidance continues evolving. New AI-specific regulations may emerge in coming years.
Organizations should expect regulatory compliance costs to increase, especially for clinical decision support tools and diagnostic AI.
Emphasis on Explainability
Black-box AI faces growing skepticism from clinicians and regulators. Demand for explainable AI increases development complexity and cost.
Building explainability into AI systems adds development complexity and cost compared to pure performance optimization. But this investment pays off in clinical adoption and regulatory acceptance.
Frequently Asked Questions
What is the average cost to implement AI in a hospital setting?
The average cost varies enormously based on scope and complexity. A focused pilot for a single use case typically costs $70,000-$200,000. Department-wide implementations run $350,000-$900,000. Enterprise AI platforms cost $1.7-3.5 million or more. These figures include software, infrastructure, integration, training, and initial deployment but not ongoing operational costs.
How long does it take to see ROI from healthcare AI?
ROI timelines depend on the use case. Administrative AI like documentation assistance can show positive returns within several months through immediate time savings. Clinical AI with quality-of-care benefits may require 12-24 months to demonstrate measurable impact. Enterprise platforms often need 18-36 months before cumulative benefits exceed cumulative costs.
Are cloud-based AI solutions cheaper than on-premises?
Cloud solutions typically have lower upfront costs but higher ongoing expenses. Over 3-5 years, total cost of ownership may be similar. Cloud works best for organizations wanting faster deployment, lower financial risk, and vendor-managed infrastructure. On-premises makes sense for organizations with data sovereignty requirements or very high usage volumes where cloud costs become prohibitive.
What are the biggest hidden costs in AI implementation?
The biggest hidden costs include data preparation (often 60-80% of project time), integration with existing systems, change management and training, ongoing model monitoring and maintenance, and regulatory compliance. Organizations frequently underestimate these by 30-50%, leading to budget overruns. Comprehensive planning that accounts for these factors improves budget accuracy.
Do smaller healthcare organizations need to spend as much on AI?
Smaller organizations can pursue AI more cost-effectively by focusing on commercial solutions rather than custom development, starting with narrow use cases, leveraging cloud deployment to avoid infrastructure costs, and partnering with vendors offering scalable pricing. Documentation AI and diagnostic AI implementations vary in cost depending on deployment method, complexity, and organizational size.
How much should organizations budget for AI maintenance annually?
Annual maintenance costs represent a significant recurring expense, typically estimated as a percentage of initial implementation costs. For a $500,000 implementation, budget accordingly for software updates, model retraining, security patches, performance monitoring, and support. More complex systems or those requiring frequent retraining may require higher budgets.
Are AI costs covered by value-based care arrangements?
Value-based care arrangements create incentives for AI adoption by allowing organizations to keep savings generated through improved efficiency and outcomes. However, the arrangements themselves rarely pay for AI implementation directly. Organizations must finance AI upfront and recoup costs through shared savings, bonus payments, or improved margins under value-based contracts. CMS initiatives like the WISeR Model and technology-enabled care programs increasingly recognize AI’s role in value-based care.
Conclusion: Making Smart AI Investment Decisions
The cost of artificial intelligence in healthcare reflects its transformative potential and substantial complexity. Implementations range from $70,000 pilots to multi-million-dollar enterprise platforms. Success requires understanding the full cost picture—not just software licensing, but infrastructure, data preparation, staffing, training, compliance, and ongoing maintenance.
Evidence from systematic reviews demonstrates that AI can achieve cost-effectiveness in clinical applications. Several interventions show incremental cost-effectiveness ratios well below accepted thresholds. But economic benefits aren’t automatic. Organizations must choose appropriate use cases, implement thoughtfully, and measure rigorously.
Smart AI investment starts with clear objectives. What clinical or operational problem needs solving? What metrics define success? How will ROI be measured? Organizations that answer these questions before selecting technology make better decisions and achieve better outcomes.
Start small. Prove value in focused pilots before scaling to enterprise deployments. Use commercial solutions when they exist rather than building custom. Invest in data quality early. Don’t skimp on change management. Budget for total cost of ownership, not just initial implementation.
The healthcare AI market continues maturing. More proven solutions exist at competitive prices. Cloud deployment reduces barriers to entry. But AI remains a significant investment requiring careful planning and realistic expectations.
For healthcare organizations ready to pursue AI, the path forward combines strategic thinking with practical execution. Understand costs comprehensively. Choose use cases with clear value propositions. Build internal capabilities gradually. Measure outcomes honestly. Adjust based on what works.
AI promises to help healthcare organizations deliver better care at lower cost. But realizing this promise requires more than enthusiasm—it demands disciplined investment, rigorous evaluation, and commitment to continuous improvement. Organizations that approach AI with financial realism and operational discipline position themselves to capture genuine value from this transformative technology.
Ready to explore AI for your healthcare organization? Start by conducting a comprehensive needs assessment, evaluating your data readiness, and identifying one high-value use case for a focused pilot. The investment required may be substantial, but the potential returns—in clinical outcomes, operational efficiency, and patient satisfaction—make AI worth serious consideration for forward-thinking healthcare leaders.
