Quick Summary: Digital transformation in healthcare involves integrating technologies like AI, IoT, electronic health records, and telemedicine to improve patient outcomes, operational efficiency, and reduce costs. Research shows that 75% of U.S. hospitals use electronic health record systems, while 65% now use AI-assisted predictive tools. Healthcare professionals and organizational readiness are critical factors for successful implementation.
Healthcare stands at a critical juncture where technology meets patient care in unprecedented ways. The COVID-19 pandemic accelerated what was already a growing trend—the integration of digital technologies into every aspect of healthcare delivery.
But here’s the thing: digital transformation isn’t just about adopting new tools. It’s about fundamentally rethinking how healthcare organizations operate, deliver care, and engage with patients.
According to research published in the International Journal of Environmental Research and Public Health (2023), the primary benefits of digital transformation include increased employee productivity, improved efficiency and effectiveness of health unit operations, and reduced operating costs. Research indicates that 75% of U.S. hospitals use electronic health record systems.
This shift affects everyone from healthcare administrators to frontline clinicians to patients themselves. And it’s only accelerating.
Understanding Digital Transformation in Healthcare
Digital transformation in healthcare refers to the comprehensive integration of digital technologies into all areas of healthcare delivery, operations, and patient engagement. It’s not simply digitizing records or adding a patient portal.
The transformation touches everything: clinical workflows, administrative processes, patient communication, data analytics, and decision-making frameworks.
Real talk: many healthcare organizations struggle with this because they treat digital transformation as an IT project rather than an organizational shift. Research from medical journals emphasizes that technology acceptance among healthcare professionals is a fundamental component of successful digital health transformation.
The World Health Organization recognizes that while digital technologies are integral to daily life and innovation is happening at unprecedented scale, the application to improve population health remains largely untapped. There’s immense scope for digital health solutions that haven’t been realized yet.
Why Traditional Healthcare Models Need Transformation
Traditional healthcare models were built around episodic, reactive care. Patients visited doctors when sick, medical records lived in filing cabinets, and coordination between providers happened through phone calls and faxed documents.
That model doesn’t work anymore. Patient expectations have changed—they expect the same digital convenience from healthcare that they get from banking, retail, and entertainment services.
Sound familiar? Healthcare costs continue rising while outcomes often lag behind other developed nations despite massive spending. In the U.S., approximately 90% of health expenses go toward disease and injury treatment rather than addressing the predisposing factors of these illnesses.
Digital transformation offers a path forward by enabling preventive care, improving coordination, reducing errors, and making healthcare more accessible.
Core Technologies Driving Healthcare Transformation
Several key technologies form the foundation of digital transformation in healthcare. These aren’t isolated tools—they work together to create interconnected systems that improve care delivery. 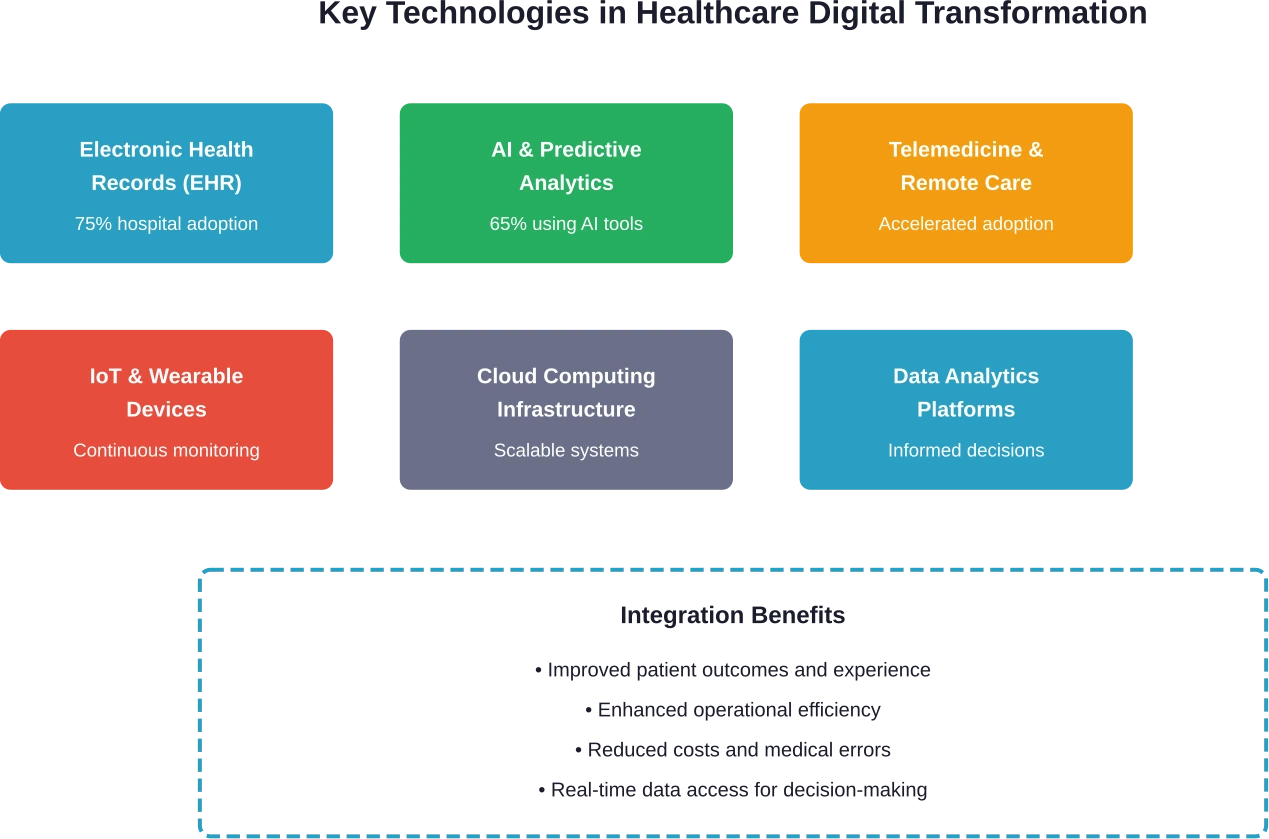
Electronic Health Records and Data Systems
Electronic health records represent the foundation of digital healthcare infrastructure. These systems centralize patient information, making it accessible to authorized providers across different locations and specialties.
The data from medical research shows that 75% of U.S. hospitals have implemented electronic health systems. That’s significant progress, but implementation quality varies widely.
EHR systems do more than store data—they enable clinical decision support, automate workflows, reduce duplicate testing, and create opportunities for data analytics. When properly implemented, they improve care coordination and patient safety.
But wait. Many healthcare professionals report that poorly designed EHR systems can actually decrease productivity and create frustration. Technology acceptance depends heavily on system usability and adequate training.
Artificial Intelligence and Predictive Analytics
AI represents one of the most transformative technologies in healthcare. According to recent data from TierPoint analysis, 65% of U.S. hospitals use AI-assisted predictive tools embedded in their EHR systems.
These tools analyze patient data to identify risk factors, predict complications, suggest treatment options, and optimize resource allocation. Machine learning algorithms can detect patterns that humans might miss.
Research published in Digital Health examined the integration of artificial intelligence and Internet of Things (AIoT) technologies in transforming healthcare delivery systems globally. The study emphasizes that comprehensive evaluation frameworks are needed to assess AIoT technological impact on sustainable healthcare delivery.
AI applications range from diagnostic imaging analysis to drug discovery to predicting patient deterioration. The technology enables more personalized, preventive care rather than reactive treatment.
Telemedicine and Remote Patient Monitoring
The COVID-19 pandemic accelerated telemedicine adoption dramatically. Virtual visits went from a convenience feature to an essential service practically overnight.
Remote patient monitoring combines telemedicine with IoT devices to track patient health metrics continuously. Wearable devices monitor heart rate, blood pressure, glucose levels, and other vital signs in real-time.
This technology is particularly valuable for managing chronic conditions, post-surgical recovery, and elderly care. Patients receive care in their homes while clinicians get continuous data streams instead of snapshots from office visits.
Research on digital health transformation highlights that the integration of wearable and information technology, virtual reality, and the Internet of Things have contributed significantly to transforming healthcare business and operations.
Cloud Computing and Infrastructure Modernization
Cloud infrastructure provides the scalability and flexibility that modern healthcare systems require. Legacy on-premises systems can’t handle the data volumes and computational demands of AI, analytics, and real-time monitoring.
Cloud platforms enable healthcare organizations to scale resources up or down based on demand, implement new applications faster, and improve disaster recovery capabilities.
Security concerns often arise with cloud adoption in healthcare, but major cloud providers now offer HIPAA-compliant infrastructure with robust security controls that often exceed what individual healthcare organizations can implement on-premises.
Key Benefits of Digital Transformation
Healthcare organizations pursue digital transformation for concrete reasons. The benefits extend across operational, clinical, and financial dimensions.
A Deloitte-Scottsdale Institute study found that 92% of survey respondents cited better patient experience as the top desired outcome from digital transformation. That’s nearly universal agreement on priorities.
Improved Patient Outcomes and Experience
Digital tools enable more accurate diagnoses, personalized treatment plans, and proactive intervention before conditions worsen. Patients can access their health information, communicate with providers, schedule appointments, and manage medications through digital platforms.
The shift from episodic to continuous care improves outcomes for chronic disease management. Remote monitoring catches problems early, reducing emergency department visits and hospitalizations.
Patient engagement increases when people have convenient access to their health data and care teams. Engaged patients typically achieve better health outcomes and experience higher satisfaction.
Enhanced Operational Efficiency
According to research published in medical journals, key benefits include increased employee productivity and improved efficiency and effectiveness of health unit operations.
Digital systems automate administrative tasks, streamline workflows, reduce duplicate data entry, and minimize errors. Staff spend less time on paperwork and more time on patient care.
Real-time data access speeds up decision-making processes. Predictive analytics help optimize staffing, supply chain management, and resource allocation.
Organizations report significant time savings in areas like appointment scheduling, insurance verification, medication reconciliation, and care coordination between departments.
Cost Reduction and Resource Optimization
The research data indicates that reducing operating costs is a primary benefit of digital transformation. Cost savings come from multiple sources: reduced errors, fewer duplicate tests, improved resource utilization, and decreased administrative burden.
Preventive care enabled by remote monitoring and data analytics costs far less than treating acute complications. Early intervention prevents expensive emergency care and hospitalizations.
Digital systems also reduce physical space requirements for records storage, decrease supply waste through better inventory management, and optimize staffing through predictive scheduling.

Plan Your AI-Driven Healthcare Transformation
Digital transformation in healthcare often involves advanced data analytics, AI-powered diagnostics, automation of administrative processes, and intelligent systems that improve patient care and operational efficiency.
Working with an experienced AI partner such as AI Superior can help healthcare organizations identify practical AI use cases, estimate implementation costs, and design solutions that integrate with existing clinical and IT systems while meeting regulatory requirements.
Their team supports healthcare organizations with:
- AI strategy and healthcare digital transformation planning
- custom AI solutions for medical and healthcare workflows
- machine learning, data infrastructure, and model deployment
If your healthcare organization is planning a digital transformation initiative, AI Superior can help design and implement AI solutions that support better patient outcomes and more efficient healthcare operations.
Implementation Challenges and Barriers
Digital transformation sounds great in theory, but healthcare organizations face substantial obstacles in practice. Understanding these challenges is essential for successful implementation.
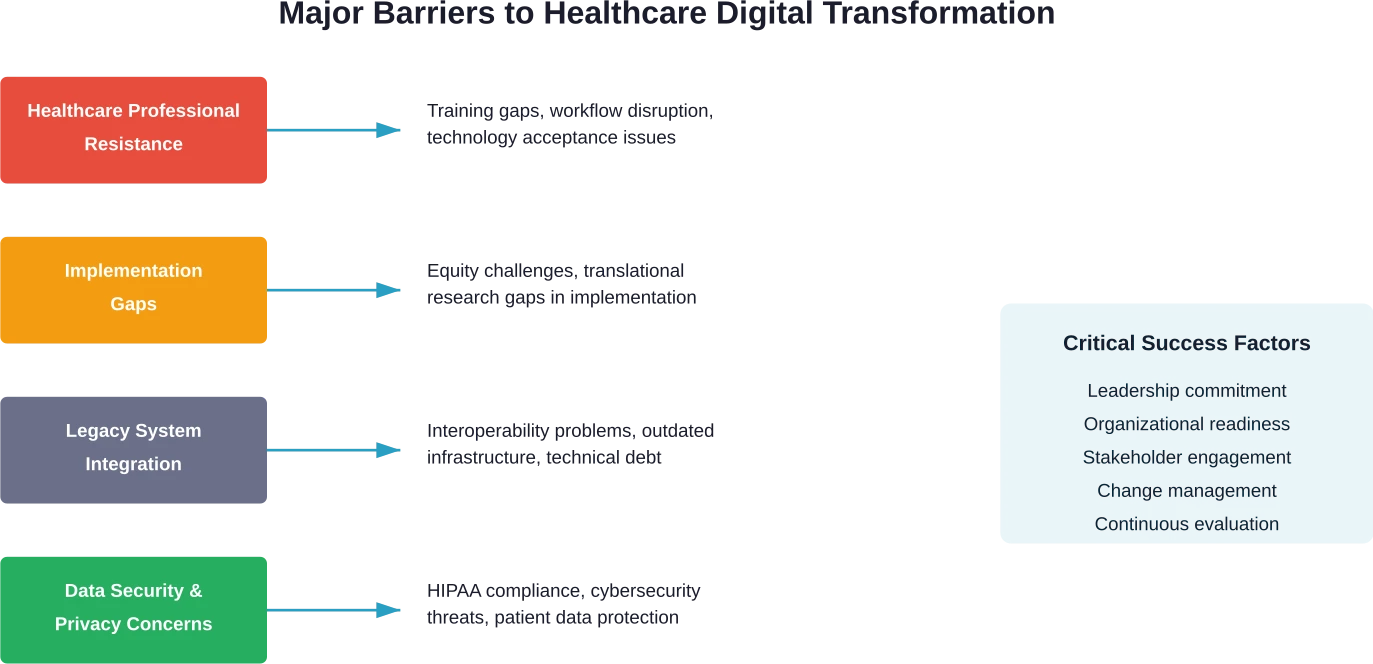
Technology Acceptance and Staff Resistance
Research published in medical journals emphasizes that healthcare professionals are a fundamental component of digital health transformation. Technology acceptance among staff determines success or failure.
Staff resistance often stems from legitimate concerns: fear that new systems will disrupt established workflows, inadequate training, or past negative experiences with poorly implemented technology.
Clinicians may worry that digital tools will distance them from patients or that they’ll spend more time documenting than providing care. These concerns require serious attention, not dismissal.
Successful organizations involve frontline staff in technology selection and implementation planning. They provide comprehensive training and ongoing support, not just a one-time orientation.
Implementation Gaps and Equity Challenges
A paper published in Clinical and Translational Science examining implementation gaps in digital health notes that the translational gap reflects fundamental challenges in how the field approaches the implementation science of digital health innovation.
The COVID-19 pandemic accelerated certain aspects of digital health adoption, particularly telemedicine. However, this rapid adoption also exposed equity gaps.
Not all patient populations have equal access to digital technologies. Rural areas may lack broadband infrastructure. Lower-income patients may not have smartphones or computers. Elderly patients may struggle with digital interfaces.
Digital transformation risks reproducing or even amplifying existing healthcare inequities if implementation doesn’t explicitly address accessibility and digital literacy across all patient populations.
Legacy Systems and Integration Issues
Most healthcare organizations operate with a patchwork of legacy systems accumulated over decades. These systems often can’t communicate with each other effectively.
Integration challenges create data silos that undermine the promise of comprehensive digital health records. Clinical staff waste time logging into multiple systems and manually transferring information between platforms.
Replacing legacy systems entirely is expensive and risky. Organizations must balance modernization with maintaining operational continuity. Phased approaches and middleware solutions help bridge old and new systems.
Data Security and Privacy Concerns
Healthcare data is a prime target for cyberattacks. Ransomware incidents have shut down hospital systems, delayed patient care, and exposed sensitive information.
Organizations must comply with regulations like HIPAA while implementing robust cybersecurity measures. The challenge intensifies as systems become more interconnected and data moves to cloud platforms.
Patient trust depends on effective data protection. High-profile breaches damage reputations and can discourage patients from sharing information necessary for quality care.
Security can’t be an afterthought—it must be built into digital transformation strategy from the beginning.
Strategic Framework for Successful Implementation
Research published in BMC Health Services Research provides recommendations to promote digital healthcare transformation in clinical practice based on an international consensus development method.
The study found that a level of accordance greater than 75% (including strongly agree and agree responses) was required to approve recommendations for digital healthcare transformation.
Leadership and Organizational Readiness
A qualitative study published in the Journal of Healthcare Leadership examined organizational factors driving the realization of digital health transformation benefits. The research emphasizes that organizational improvements and changes in system capabilities are required to assist in realizing benefits.
Leadership commitment means more than budget allocation. Leaders must champion cultural change, communicate vision clearly, and model adoption of new technologies.
Organizational readiness assessment identifies gaps in infrastructure, skills, processes, and culture before launching major initiatives. Organizations can’t transform what they don’t understand.
According to job posting data analysis from Northeastern Online, there’s been a 35.5% growth in health management careers from 2017 to 2022. Healthcare facilities need professionals with business or management backgrounds to lead transformative initiatives alongside technology specialists.
Stakeholder Engagement and Change Management
Successful digital transformation requires engagement from all stakeholders: clinicians, nurses, administrative staff, IT teams, and patients.
Each group has different needs, concerns, and perspectives. Implementation plans must address these diverse viewpoints rather than imposing a one-size-fits-all approach.
Change management processes help people transition from current state to future state. Communication, training, support systems, and feedback mechanisms are essential components.
Organizations that treat digital transformation as a technical project tend to fail. Those that recognize it as organizational change involving people, processes, and culture alongside technology tend to succeed.
Phased Implementation and Continuous Evaluation
Attempting to transform everything simultaneously is a recipe for disaster. Phased approaches allow organizations to learn, adjust, and build momentum.
Starting with pilot projects in specific departments or with particular technologies provides valuable lessons without organization-wide disruption.
Continuous evaluation measures whether digital transformation is achieving desired outcomes. Are patient outcomes improving? Is efficiency increasing? What problems have emerged?
Organizations using frameworks like the Baldrige Excellence Framework have successfully guided digital health transformations through systematic assessment and improvement, with the program being in place for more than 20 years.
Real-World Applications and Use Cases
Digital transformation manifests differently across various healthcare settings. Looking at specific applications helps clarify what transformation looks like in practice.
| Application Area | Digital Technologies Used | Primary Benefits | Implementation Considerations |
|---|---|---|---|
| Chronic Disease Management | Remote monitoring, wearables, telemedicine, AI analytics | Reduced hospitalizations, improved outcomes, patient empowerment | Patient engagement, data integration, clinician workflows |
| Emergency Department Operations | Predictive analytics, real-time dashboards, automated triage | Reduced wait times, optimized staffing, better resource allocation | System integration, staff training, process redesign |
| Surgical Services | Robotic surgery, AI imaging, digital OR integration | Precision, reduced complications, faster recovery | High costs, specialized training, technical support |
| Population Health | Big data analytics, risk stratification, outreach automation | Preventive care, targeted interventions, cost reduction | Data quality, interoperability, privacy protection |
| Clinical Research | Electronic data capture, AI analysis, virtual trials | Faster enrollment, real-world evidence, reduced costs | Regulatory compliance, data standards, participant engagement |
Chronic Disease Management and Remote Care
Chronic conditions like diabetes, heart disease, and hypertension account for the majority of healthcare costs. Digital tools enable continuous monitoring and management between office visits.
Patients use connected devices to track glucose levels, blood pressure, weight, and activity. Data flows automatically to care teams who can intervene when concerning trends emerge.
This approach prevents complications that lead to emergency department visits and hospitalizations. Patients report feeling more supported and engaged in their care.
Predictive Analytics for Resource Management
Hospitals use predictive analytics to forecast patient volumes, identify patients at risk for complications, and optimize resource allocation.
AI models predict which patients are likely to deteriorate, which emergency department visits could escalate, and where capacity constraints will emerge.
These insights enable proactive staffing adjustments, earlier interventions, and better utilization of expensive resources like ICU beds and surgical suites.
Telemedicine and Virtual Care Delivery
Virtual visits have evolved from basic video calls to comprehensive care platforms integrating scheduling, documentation, prescriptions, and follow-up.
Specialty consultations reach rural areas that lack local specialists. Mental health services expand access for patients who face barriers to in-person appointments.
Hybrid models combine virtual and in-person care based on patient needs and preferences. This flexibility improves access while maintaining quality.
Future Trends and Emerging Technologies
Digital transformation in healthcare continues evolving rapidly. Several emerging trends will shape the next phase of change.
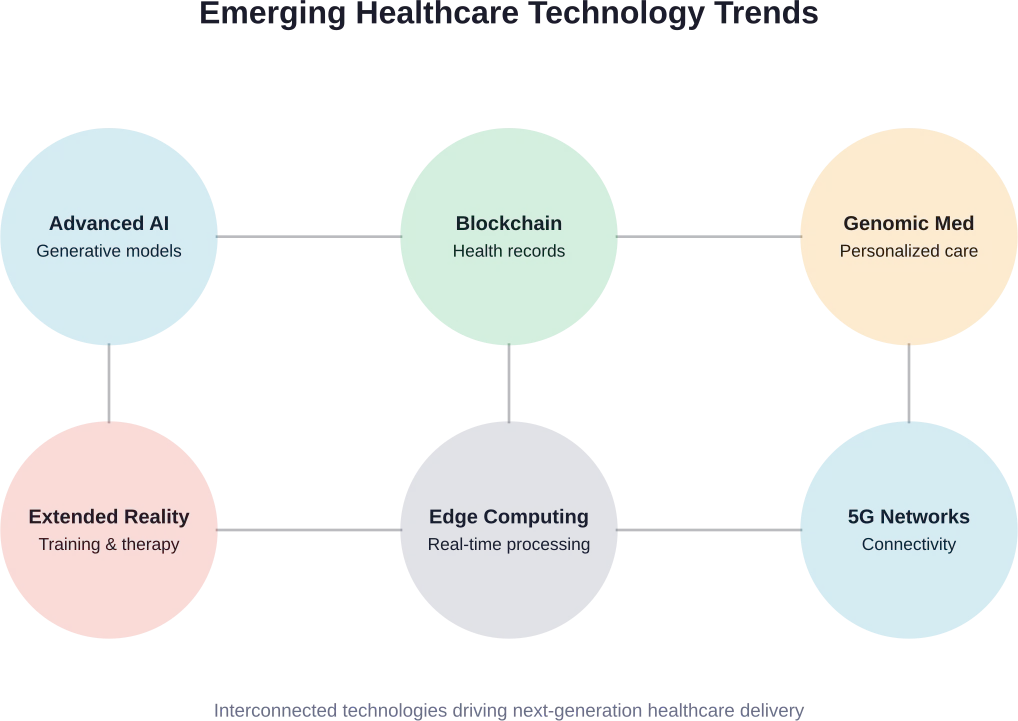
Advanced AI and Machine Learning Applications
AI capabilities continue advancing rapidly. Generative AI models can now assist with clinical documentation, patient education materials, and treatment planning.
Machine learning algorithms are becoming more sophisticated at analyzing medical imaging, predicting disease progression, and identifying optimal treatment protocols for individual patients.
The integration of AI with genomic data enables truly personalized medicine based on individual genetic profiles, lifestyle factors, and environmental exposures.
Blockchain for Health Records and Data Security
Blockchain technology offers potential solutions for health information exchange, data security, and patient control over medical records.
Decentralized systems could enable patients to grant temporary access to their health data across different providers while maintaining a complete audit trail.
Implementation challenges remain around scalability, interoperability standards, and regulatory frameworks, but pilot projects show promise.
Extended Reality in Medical Training and Treatment
Virtual reality and augmented reality applications are expanding in medical education, surgical planning, pain management, and mental health treatment.
Surgeons can practice complex procedures in VR environments. Patients can use VR for distraction during painful procedures or as part of physical rehabilitation programs.
AR can overlay digital information onto physical environments, assisting surgeons during operations or helping nurses locate veins for IV placement.
Building a Digital-First Healthcare Culture
Technology alone doesn’t create transformation. Organizational culture determines whether digital tools deliver their potential value.
Developing Digital Competencies
Healthcare professionals need new skills to work effectively in digital environments. Digital literacy, data interpretation, and technology troubleshooting become essential competencies.
Organizations must invest in training programs that go beyond basic system operation to develop strategic thinking about how digital tools can improve care delivery.
According to research on organizational factors driving digital health transformation, changes in system capabilities and management skills are required to realize transformation benefits.
Patient Engagement and Digital Health Literacy
Digital transformation requires engaged patients who actively participate in their care using digital tools.
Not all patients start with equal digital health literacy. Education programs, intuitive interfaces, and support resources help patients become comfortable with patient portals, telemedicine platforms, and remote monitoring devices.
Organizations should design digital services with diverse patient populations in mind, ensuring accessibility for people with disabilities, limited English proficiency, or low digital literacy.
Fostering Innovation and Experimentation
Healthcare organizations traditionally emphasize standardization and risk mitigation. Digital transformation requires balancing these important values with space for innovation.
Creating innovation labs, pilot programs, and partnerships with technology companies allows experimentation without disrupting core operations.
Learning from both successes and failures accelerates progress. Organizations that punish failure discourage the experimentation necessary for innovation.
Measuring Success and ROI
Organizations need clear metrics to evaluate whether digital transformation is delivering expected benefits.
| Measurement Category | Key Metrics | Data Sources |
|---|---|---|
| Clinical Outcomes | Readmission rates, complication rates, mortality rates, patient safety indicators | EHR systems, quality registries, patient records |
| Patient Experience | Satisfaction scores, Net Promoter Score, access metrics, engagement levels | Patient surveys, portal analytics, appointment data |
| Operational Efficiency | Length of stay, throughput times, staff productivity, resource utilization | Operations systems, scheduling platforms, time studies |
| Financial Performance | Cost per case, revenue cycle metrics, supply costs, staffing costs | Financial systems, billing platforms, budget reports |
| Staff Satisfaction | Engagement scores, turnover rates, system usability ratings | Employee surveys, HR systems, usability testing |
Clinical Quality and Patient Safety Metrics
The ultimate measure of healthcare transformation is whether patient outcomes improve. Tracking clinical quality metrics before and after digital implementations shows impact.
Relevant metrics include complication rates, hospital-acquired infection rates, medication errors, falls, and condition-specific outcomes.
Digital tools should reduce errors and improve adherence to evidence-based protocols. If quality metrics don’t improve, implementation needs reassessment.
Financial and Operational Indicators
Organizations track return on investment through operational efficiency gains and cost reductions.
Reduced length of stay, fewer duplicate tests, optimized staffing, and decreased supply waste all contribute to financial benefits.
Digital transformation requires significant upfront investment. ROI calculations should include both direct cost savings and value from improved outcomes and patient satisfaction.
Technology Adoption and Utilization Rates
Even the best technology delivers no value if people don’t use it. Tracking adoption rates among staff and patients identifies training needs and usability problems.
Utilization metrics for patient portals, telemedicine platforms, and clinical decision support tools show whether digital services are reaching intended users.
Low adoption rates signal problems that need addressing—whether related to design, training, communication, or the value proposition itself.
Regulatory and Compliance Considerations
Healthcare operates in a heavily regulated environment. Digital transformation must address compliance requirements from the start.
HIPAA and Data Privacy Requirements
Any system that stores, transmits, or processes protected health information must comply with HIPAA security and privacy rules.
Organizations must implement technical safeguards, administrative policies, and physical security measures. Business associate agreements are required for vendors who handle health data.
Privacy impact assessments should be conducted before implementing new digital systems to identify and mitigate risks.
Interoperability and Data Exchange Standards
Regulations increasingly require healthcare organizations to support data portability and patient access to health information.
Standards like HL7 FHIR enable data exchange between different systems. Organizations must implement APIs that allow patients to access their data through third-party applications.
Achieving true interoperability remains challenging despite regulatory mandates. Technical standards, business models, and competitive concerns all create friction.
Clinical Validation and FDA Oversight
Digital health tools that diagnose, treat, or prevent disease may qualify as medical devices subject to FDA regulation.
Organizations must understand which digital tools require regulatory clearance and ensure vendors have obtained necessary approvals.
Clinical validation demonstrates that digital tools perform as intended and improve outcomes. Evidence requirements vary based on risk level and intended use.
Frequently Asked Questions
What is digital transformation in healthcare?
Digital transformation in healthcare is the comprehensive integration of digital technologies into all aspects of healthcare delivery, operations, and patient engagement. It goes beyond simply digitizing records to fundamentally rethinking how organizations operate, deliver care, and interact with patients. Key technologies include electronic health records, artificial intelligence, telemedicine, IoT devices, cloud computing, and data analytics platforms working together to improve outcomes and efficiency.
How much does digital transformation cost for healthcare organizations?
Costs vary dramatically based on organization size, existing infrastructure, scope of transformation, and chosen technologies. Large hospital systems may invest tens of millions in comprehensive EHR implementations, while smaller practices might start with modest telemedicine platforms costing thousands. Organizations should focus on phased approaches that demonstrate ROI before expanding investment. Check with vendors for current pricing as costs change frequently based on organization size and requirements.
What are the biggest barriers to healthcare digital transformation?
The major barriers include staff resistance and technology acceptance issues, implementation gaps that create equity challenges, legacy system integration problems, data security and privacy concerns, inadequate training and digital literacy, insufficient leadership commitment, and the challenge of balancing innovation with regulatory compliance. Research shows that healthcare professional engagement is the most critical factor—technology fails without user adoption.
How long does healthcare digital transformation take?
Digital transformation is an ongoing journey rather than a destination with a fixed timeline. Major EHR implementations typically take 18-36 months from selection to full deployment. However, comprehensive organizational transformation involving culture change, process redesign, and multiple technology implementations may take 5-10 years. Organizations see best results with phased approaches that deliver incremental value while building toward long-term vision.
How does digital transformation improve patient outcomes?
Digital transformation improves outcomes through multiple mechanisms: AI-assisted diagnostics catch diseases earlier and more accurately, remote monitoring enables proactive intervention before conditions deteriorate, clinical decision support reduces errors and improves adherence to evidence-based protocols, care coordination platforms improve communication between providers, and data analytics identify high-risk patients for targeted interventions. Research shows these technologies collectively reduce complications, hospitalizations, and mortality when implemented effectively.
What role does AI play in healthcare digital transformation?
AI serves multiple critical functions in healthcare transformation. According to recent data from TierPoint analysis, 65% of U.S. hospitals use AI-assisted predictive tools embedded in their EHR systems. Applications include analyzing medical imaging for diagnosis, predicting patient deterioration or readmission risk, optimizing treatment plans based on patient characteristics, automating administrative tasks, and discovering patterns in large datasets that inform population health strategies. AI enables more personalized, preventive care rather than reactive treatment.
How can small healthcare practices implement digital transformation?
Small practices should start with high-impact, manageable initiatives rather than attempting comprehensive transformation simultaneously. Priorities might include implementing a cloud-based EHR if still using paper records, adding a patient portal for appointment scheduling and communication, incorporating telemedicine capabilities for appropriate visits, and using practice management software to automate administrative workflows. Many vendors offer affordable, scalable solutions designed specifically for small practices. Focus on technologies that directly address the practice’s biggest pain points and demonstrate clear value before expanding.
Moving Forward with Digital Healthcare
Digital transformation represents both enormous opportunity and significant challenge for healthcare organizations. The evidence is clear: properly implemented digital technologies improve patient outcomes, enhance operational efficiency, and reduce costs.
But technology alone doesn’t create transformation. Success requires leadership commitment, organizational readiness, stakeholder engagement, cultural change, and continuous evaluation.
The pace of technological innovation will only accelerate. Healthcare organizations that develop digital capabilities, foster innovation cultures, and build transformation expertise will be best positioned to deliver high-quality, accessible, affordable care in an increasingly digital world.
The question isn’t whether to pursue digital transformation—it’s how to do it effectively while maintaining focus on the ultimate goal: better health outcomes for the patients and communities healthcare organizations serve.
Organizations beginning their digital transformation journey should start with clear assessment of current state, specific goals tied to patient and operational outcomes, stakeholder engagement across all levels, phased implementation plans that build momentum, and measurement systems that track progress and inform adjustments.
The transformation journey is complex, but the destination—a healthcare system that’s more effective, efficient, and equitable—makes the effort worthwhile.
