Quick Summary: AI will not replace surgeons entirely, but rather transform their role through advanced assistance and collaboration. Current AI and robotic systems excel at specific surgical tasks like precision cutting, imaging analysis, and preoperative planning, but lack the judgment, adaptability, and human skills required for complete autonomy. The future of surgery lies in human-AI partnerships where technology enhances surgical capabilities while surgeons maintain oversight, decision-making authority, and patient care responsibilities.
The question of whether artificial intelligence will replace surgeons has moved from science fiction to serious medical discussion. With robotic systems performing complex procedures and machine learning algorithms predicting surgical outcomes with remarkable accuracy, it’s natural to wonder about the future of human surgeons.
But here’s the thing—the reality is far more nuanced than the headlines suggest.
AI is already transforming surgery in profound ways. According to the American College of Surgeons, AI represents “an avalanche heading for the healthcare industry,” with applications growing rapidly across surgical specialties. Yet despite these advances, the complete replacement of human surgeons remains a distant prospect, constrained by technical limitations, patient psychology, and the irreplaceable nature of human judgment.
This article examines what AI can actually do in surgery today, where the technology falls short, and what the future likely holds for the relationship between artificial intelligence and surgical practice.
The Current State of AI in Surgical Practice
AI has already established a significant foothold in operating rooms worldwide, though not in the ways many people imagine.
Rather than autonomous robots performing entire procedures independently, current applications focus on specific tasks where computational precision offers clear advantages over human capabilities alone.
Robotic Surgery Systems Today
The da Vinci Surgical System represents the most widely recognized surgical robot, used in specialties including urology, gynecology, and cardiothoracic surgery. These systems don’t operate independently—they’re essentially sophisticated tools that translate a surgeon’s hand movements into precise instrument actions.
According to research from The University of Chicago Medicine, robotic endoscopic mitral valve procedures have demonstrated excellent 30-day surgical outcomes, reinforcing the growing role of minimally invasive robotic approaches.
That said, there’s a catch. Research published by the American College of Surgeons shows that claims-based studies actually underestimate the adoption of robotic surgery due to low sensitivity of billing codes. The technology is more prevalent than administrative data suggests.
AI in Preoperative Planning
This is where AI truly shines today.
In total knee arthroplasty, machine learning algorithms can predict postoperative complications such as transfusion needs with high accuracy, achieving AUC values up to 0.842, according to research published in Knee Surgery and Related Research. Deep learning techniques facilitate 3D anatomical reconstruction and implant size prediction, with some models achieving over 90% accuracy.
A systematic review published in the European Journal of Orthopaedic Surgery found that AI models for predicting total knee arthroplasty component sizes showed femoral component accuracy ranging from 88.3% to 99.7% within one size deviation, while tibial component sizing exhibited accuracy ranging from 90% to 99.9% ± 1 size.
These aren’t trivial improvements. Accurate preoperative planning reduces surgical time, minimizes complications, and improves patient outcomes.
Imaging Analysis and Anatomical Recognition
Modern AI algorithms utilize deep learning techniques to automatically generate highly accurate three-dimensional models from CT and MRI scans. According to research on AI-enhanced surgical decision-making in orthopedics, these AI-driven systems help surgeons perform highly precise interventions.
The technology excels at pattern recognition tasks that would take human radiologists significantly longer to complete. But recognition isn’t the same as interpretation—understanding what those patterns mean in the context of a specific patient still requires clinical expertise.
Postoperative Patient Support
AI chatbots have been trialed for postoperative patient questions, particularly in obstetrics. According to the American College of Surgeons, when patients wake at 1:00 in the morning two days after surgery wondering if a symptom is normal, they can contact a chatbot for immediate guidance. Studies show 96% of patients viewed this tool positively.
However, research examining patient questions after knee arthroplasty found that over 90% of patients surveyed were uncertain about trusting AI to answer their postoperative questions, despite the chatbot providing appropriate responses as determined by fellowship-trained surgeons.

End-to-End AI Support With AI Superior
AI Superior works across the full lifecycle of AI projects, from early-stage assessment to deployment. The focus is on building solutions that can operate reliably once integrated into real systems.
Need Support Across an AI Project?
AI Superior can help with:
- building AI applications from concept to deployment
- defining technical direction and project scope
- integrating AI into operational environments
👉 Contact AI Superior to discuss your project, data, and implementation approach
Why Complete Replacement Remains Unlikely
The gap between what AI can do and what’s required to replace surgeons entirely is vast—and some of those gaps may be fundamentally unbridgeable.
The Self-Driving Car Problem
Here’s a useful comparison: if companies with billions in research funding still struggle to get autonomous vehicles to reliably identify a plastic bag versus a pedestrian, imagine the challenge inside the human body.
Surgery isn’t like navigating a highway. Anatomy shifts, bleeds, hides behind other structures, and varies wildly between patients. During operations, surgeons constantly make judgment calls: Is that a small vessel or a major branch? Is this a nerve that must be protected? Is that fascia or something more critical hiding underneath?
AI vision systems today simply aren’t close to matching human perception in that dynamic, unpredictable environment. The variability is too high, the stakes too severe, and the edge cases too numerous.
Patient Trust and Acceptance
Even if the technology existed, would patients accept it?
Research shows that approximately 30% of patients express distrust toward health information produced by generative AI itself. Interestingly, a majority (64%) trust their doctors to use AI responsibly to improve their care, according to data published by the American College of Surgeons.
People are already uneasy about riding in driverless cars. Being operated on by an autonomous system? That’s an entirely different psychological threshold.
According to data cited by the American College of Surgeons, 60% of Americans would be uncomfortable with healthcare providers relying on AI in their own medical care. This isn’t irrational technophobia—it reflects legitimate concerns about accountability, safety, and the irreplaceable value of human judgment in high-stakes situations.
Regulatory and Liability Challenges
Who’s liable when an autonomous surgical system makes a mistake?
Current regulatory frameworks aren’t remotely prepared for fully autonomous surgery. Medical device approval processes require extensive validation, and the legal frameworks for algorithmic medical decision-making remain underdeveloped.
These aren’t just bureaucratic obstacles. They reflect fundamental questions about responsibility, informed consent, and patient rights that society hasn’t yet answered.
The Irreplaceable Human Elements
Surgery involves far more than technical execution.
Surgeons provide preoperative counseling, helping patients understand risks and make informed decisions. They adapt plans mid-procedure when unexpected findings emerge. They communicate with families during long operations. They manage postoperative complications that don’t fit textbook patterns.
These skills involve empathy, communication, ethical reasoning, and creative problem-solving—capabilities that remain firmly in the domain of human intelligence.
| Capability | Current AI Performance | Human Surgeon Performance | Gap Status |
|---|---|---|---|
| Imaging analysis and pattern recognition | Excellent (90%+ accuracy for specific tasks) | Very good but slower | AI advantage for specific tasks |
| Preoperative planning and prediction | Very good (AUC up to 0.842 for complications) | Good but variable | AI augments effectively |
| Precise, repetitive movements | Excellent (robotic systems) | Good but fatigue-prone | AI/robotic advantage |
| Adaptation to unexpected findings | Poor to nonexistent | Excellent | Significant human advantage |
| Complex clinical judgment | Limited to narrow contexts | Excellent when experienced | Significant human advantage |
| Patient communication and empathy | Poor (chatbots have limitations) | Variable but uniquely human | Fundamental human advantage |
| Ethical decision-making | Cannot perform independently | Essential surgical skill | Unbridgeable gap |
What AI Is Actually Changing in Surgery
While complete replacement isn’t on the horizon, AI is fundamentally changing how surgery works—just not in the ways headlines suggest.
Enhanced Surgical Precision
Robotic systems that assist with surgical tasks provide measurable improvements in precision. These aren’t autonomous robots—they’re advanced tools that amplify human capabilities.
In orthopedic surgery, robotic arms help prepare bone cuts with perfect alignment. Navigation systems improve accuracy. AI highlights nerves or vessels on screen during procedures. Planning tools personalize surgical strategy based on individual patient anatomy.
According to research published in medical journals examining AI in total knee arthroplasty, these technologies enable analysis and optimization across the entire surgical workflow, from patient selection through recovery.
Predictive Analytics for Better Outcomes
Machine learning excels at identifying patterns in large datasets that humans might miss.
A scoping review of AI applications in predicting open-heart surgery outcomes examined 64 studies. The most frequently employed algorithm was logistic regression (used in 41 studies), followed by random forest in 38 studies. These predictive models help identify high-risk patients and optimize perioperative care.
This represents a shift from reactive to proactive surgical care—anticipating problems before they occur rather than responding after they develop.
Reduced Administrative Burden
A significant portion of surgical workflow involves documentation, coding, scheduling, and other administrative tasks.
AI systems can automate much of this work, freeing surgeons to focus on patient care. Natural language processing can generate operative reports from voice recordings. Scheduling algorithms can optimize operating room utilization. Billing systems can automatically code procedures based on operative notes.
These applications don’t replace surgeons—they give them more time to be surgeons.
Democratization of Expertise
AI-powered decision support systems can help less experienced surgeons access the accumulated knowledge of thousands of previous cases.
Virtual tumor boards using AI assistance provide access to multidisciplinary cancer care for rural patients who might otherwise lack specialist input. Real-time guidance systems can flag potential complications before they become critical.
This doesn’t eliminate the need for expertise—it distributes it more equitably.
The Future of Human-AI Collaboration in Surgery
So what does the future actually look like?
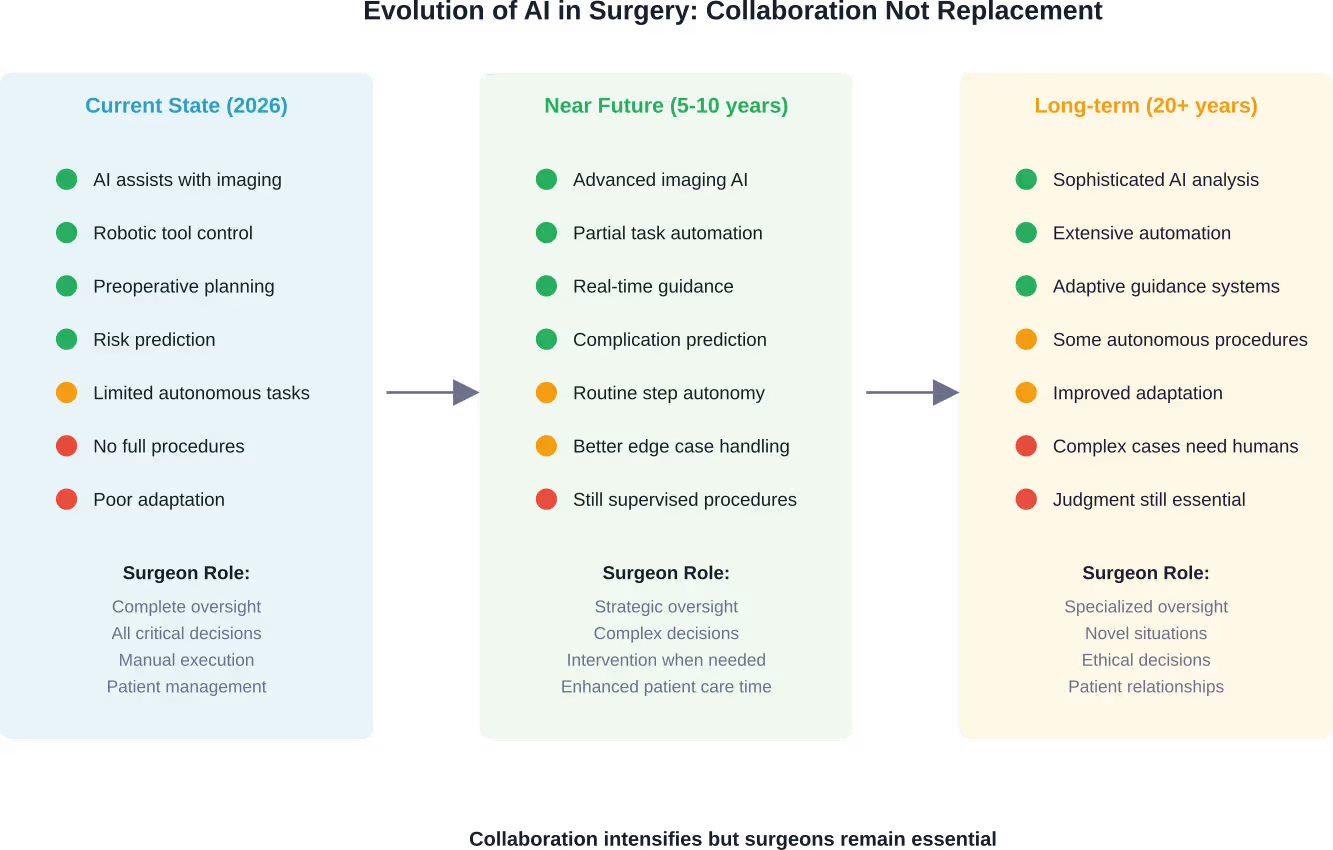
Most experts envision a collaborative model where AI handles specific tasks exceptionally well while human surgeons maintain oversight, make critical decisions, and provide the judgment that technology cannot replicate.
The Copilot Model
Think of AI as a copilot rather than a replacement pilot.
Commercial aviation provides a useful analogy. Modern aircraft have extensive automation—autopilot systems can handle takeoff, navigation, and landing under many conditions. Yet we still train pilots extensively and require them in the cockpit.
Why? Because automation handles routine situations brilliantly but struggles with edge cases, system failures, and situations that don’t match its training data. Human judgment remains essential.
The same principle applies to surgery. AI will handle increasingly sophisticated tasks, but someone needs to supervise, intervene when things go wrong, and make decisions that fall outside algorithmic parameters.
Evolving Surgical Training
If AI handles more routine tasks, surgical training will need to evolve.
Future surgeons will need deep understanding of AI systems—their capabilities, limitations, and failure modes. They’ll need to know when to trust algorithmic recommendations and when to override them. They’ll need skills in supervising automated systems and intervening when necessary.
But they’ll still need traditional surgical skills, because someone must be able to take over when technology fails. Just as pilots still train for manual flight despite extensive automation, surgeons will train for manual surgery despite AI assistance.
Research from the AI Centre of Excellence suggests that 40% of the workforce needs reskilling and upskilling to perform their current role in the next one to three years as businesses transform with AI integration. Surgery won’t be exempt from this trend.
Economic and Access Implications
The costs associated with robotic surgery systems present significant barriers to widespread adoption.
Initial system purchases can range from $1 million to over $2.5 million per unit. Annual maintenance and per-procedure costs contribute significantly to overall expenses. These figures can limit accessibility of robotic surgery in resource-constrained environments.
However, as technology matures and competition increases, costs typically decline. AI software assistance may prove more economically accessible than robotic hardware, potentially democratizing access to surgical expertise rather than concentrating it.
Specific Surgical Specialties and AI Impact
The impact of AI varies considerably across surgical specialties based on the nature of procedures and the degree of standardization possible.
Orthopedic Surgery
Orthopedics has seen particularly rapid AI integration, especially in joint replacement procedures.
The high degree of anatomical standardization in procedures like total knee arthroplasty makes them well-suited for AI assistance. Preoperative planning, implant sizing, and intraoperative guidance all benefit from computational precision.
Research published in the Journal of Orthopaedic Sports Medicine provides an overview of AI applications across the entire knee arthroplasty workflow from preoperative assessment through postoperative recovery. Both ChatGPT and nurses provided appropriate answers to frequently asked patient questions, as determined by fellowship-trained surgeons, though patient trust remains an issue.
Cardiac Surgery
Cardiac surgery combines highly technical precision requirements with life-threatening time pressure—an area where AI assistance offers clear value.
The American College of Surgeons reported that robotic endoscopic mitral valve procedures have demonstrated excellent 30-day surgical outcomes. A scoping review examining AI in predicting open-heart surgery outcomes found that 89.06% of studies were retrospective, indicating the field is still in early validation stages.
Predictive models help identify patients at high risk for complications, enabling optimized perioperative management.
General Surgery
General surgery encompasses enormous procedural variety, making complete standardization difficult.
AI applications focus primarily on specific tasks: identifying anatomical structures during laparoscopic procedures, predicting surgical site infections, optimizing patient selection for specific approaches.
The variability inherent in general surgery—different pathologies, patient anatomies, and emergency situations—makes full automation particularly challenging.
Barriers That May Never Fully Resolve
Some obstacles to complete surgeon replacement aren’t merely technical challenges waiting for better algorithms—they’re fundamental limitations.
The Black Box Problem
Many advanced AI systems, particularly deep learning models, function as “black boxes.” They produce accurate predictions but can’t explain their reasoning in ways humans can validate.
In surgery, this creates serious problems. When an AI system recommends a particular approach, surgeons need to understand why. If complications arise, they need to understand what the system was “thinking.” Unexplainable recommendations are difficult to integrate into clinical decision-making, especially in high-stakes situations.
Edge Cases and Novel Situations
AI systems train on historical data. They excel at situations similar to their training examples. They struggle with truly novel circumstances.
Surgery regularly presents situations that don’t match historical patterns—unusual anatomical variants, unexpected intraoperative findings, rare complications, interactions between multiple pathologies.
Human surgeons reason through these situations using fundamental principles, creative problem-solving, and analogical thinking. AI systems lack these capabilities.
The Empathy Gap
Medicine isn’t purely technical—it’s fundamentally about caring for human beings in vulnerable situations.
Patients need explanations they can understand. They need reassurance. They need someone who acknowledges their fears and hopes. They need advocates who will fight for their interests.
These aren’t peripheral nice-to-haves—they’re core elements of medical care that affect compliance, outcomes, and patient satisfaction. AI chatbots can provide information, but they can’t provide genuine empathy.
What This Means for Patients
For patients facing surgery, what does the AI revolution actually mean?
Better Outcomes Through Enhanced Precision
The most immediate benefit is improved surgical precision and planning.
AI-assisted preoperative planning helps surgeons prepare more thoroughly. Intraoperative guidance systems reduce errors. Predictive analytics identify high-risk patients who need extra precautions. Postoperative monitoring catches complications earlier.
These improvements translate to better outcomes, fewer complications, and faster recovery.
More Informed Consent
AI-powered risk prediction provides more accurate information for consent discussions.
Rather than general population statistics, surgeons can provide personalized risk estimates based on individual patient characteristics. This enables more informed decision-making about whether to proceed with surgery and which approach to choose.
Continued Need for Human Surgeons
Patients can expect their surgeons to use increasingly sophisticated AI tools, but they shouldn’t expect—or necessarily want—fully autonomous surgical systems.
The value of human judgment, empathy, and adaptability in surgical care remains irreplaceable. The goal should be surgeons enhanced by AI, not replaced by it.
| Patient Concern | AI Impact | Surgeon Role |
|---|---|---|
| Surgical precision and accuracy | Improved through robotic assistance and navigation | Oversees and controls AI-assisted systems |
| Risk of complications | Better prediction (AUC up to 0.842) enables prevention | Interprets predictions and adjusts care plans |
| Personalized treatment planning | AI analyzes imaging and predicts optimal approaches | Makes final decisions based on clinical judgment |
| Postoperative support | Chatbots provide 24/7 information access | Handles complex questions and complications |
| Trust and communication | Limited—64% trust doctors who use AI appropriately | Provides empathy, explanations, and advocacy |
| Handling unexpected problems | Poor adaptation to novel situations | Essential for managing surgical surprises |
The Realistic Timeline
When might we actually see autonomous surgical systems, if ever?
Near-Term (Next 5 Years)
Expect continued incremental improvements in AI assistance for specific surgical tasks.
Imaging analysis will become more sophisticated. Robotic systems will handle more routine procedural steps with minimal human input. Predictive analytics will improve. Decision support systems will become more integrated into surgical workflow.
But surgeons will remain firmly in control, making critical decisions and performing complex portions of procedures manually.
Medium-Term (5-15 Years)
Some highly standardized procedures in controlled environments might see increased autonomy for specific steps.
Think of routine portions of common procedures where the anatomy is predictable and the task is repetitive. AI systems might handle these segments independently while surgeons supervise and perform more complex elements.
Surgical training will evolve to incorporate AI supervision skills. Regulatory frameworks will develop for semi-autonomous systems.
Long-Term (15+ Years)
This is where predictions become speculation.
Potentially, some straightforward procedures in ideal conditions might be performed with minimal human intervention—though still under human supervision. But complex surgeries, emergency procedures, and cases involving unusual anatomy will continue requiring human surgeons.
The more realistic long-term vision isn’t surgeonless operating rooms—it’s dramatically enhanced human-AI collaboration where technology handles routine elements while humans focus on judgment, adaptation, and patient care.
Preparing for an AI-Enhanced Surgical Future
The surgical community is actively preparing for increased AI integration.
Regulatory Development
The Joint Commission and other regulatory bodies are developing frameworks for AI in healthcare settings. According to the American College of Surgeons, Accreditation 360—supported by data, analytics, and benchmarking tools—is designed to elevate clinical outcomes and reduce administrative burden.
These frameworks will need to balance innovation with patient safety, encourage beneficial applications while preventing premature deployment of unvalidated systems.
Education and Training
Medical schools and surgical residency programs are incorporating AI education into curricula.
Future surgeons need understanding of machine learning principles, AI system limitations, and appropriate use of algorithmic decision support. They need skills in human-AI collaboration and the judgment to know when to trust or override AI recommendations.
Ethical Guidelines
Professional organizations are developing ethical guidelines for AI use in surgery.
These address questions of informed consent, liability allocation, data privacy, algorithmic bias, and maintaining patient-centered care in increasingly automated environments.
Key Takeaways
After examining the evidence, several conclusions emerge clearly:
AI will not replace surgeons in the foreseeable future. The technical challenges are substantial, patient acceptance is limited, regulatory frameworks are underdeveloped, and the irreplaceable human elements of surgery—judgment, empathy, adaptation—remain beyond AI capabilities.
AI is transforming surgery in meaningful ways. Improved preoperative planning, enhanced intraoperative precision, better risk prediction, and streamlined administrative work are already improving outcomes and efficiency.
The future is collaborative. The most likely trajectory involves increasingly sophisticated AI systems handling specific tasks while human surgeons maintain oversight, make critical decisions, and provide the judgment and empathy that technology cannot replicate.
Different specialties will see different impacts. Highly standardized procedures like joint replacement will see more AI integration than highly variable fields like trauma surgery or complex oncologic procedures.
Patient trust matters enormously. Even if technology advanced more rapidly than expected, patient acceptance would likely lag. Most people want human surgeons using AI tools, not AI systems replacing human surgeons.
The goal should be enhancement, not replacement. The most beneficial path forward isn’t eliminating human surgeons—it’s augmenting their capabilities so they can provide better, safer, more personalized care.
Frequently Asked Questions
Will AI completely replace surgeons in the next 10 years?
No, complete replacement of surgeons is extremely unlikely within the next decade. While AI will handle increasingly sophisticated assistance tasks, the complexity of surgical decision-making, the need for adaptation to unexpected findings, and the importance of human judgment mean surgeons will remain essential. Current AI systems excel at specific narrow tasks but lack the general intelligence required for full surgical autonomy.
Are robotic surgeries performed without human surgeons?
No, current robotic surgery systems like the da Vinci are entirely controlled by human surgeons. These robots don’t operate autonomously—they translate a surgeon’s hand movements into precise instrument actions. The surgeon remains in complete control throughout the procedure, making all decisions and performing all critical tasks through the robotic interface.
What surgical tasks can AI currently perform independently?
AI can independently perform imaging analysis, generate 3D anatomical models from scans, predict surgical complications with high accuracy, recommend optimal implant sizes, and provide postoperative information to patients through chatbots. However, all clinical applications require human oversight and validation. No AI systems currently perform complete surgical procedures autonomously.
Do patients trust AI in surgery?
Patient trust is mixed and context-dependent. Research shows that approximately 30% of patients express distrust toward health information produced by AI alone, while 64% trust their doctors to use AI appropriately. Over 90% of patients surveyed were uncertain about trusting AI to answer postoperative questions independently. Most patients prefer human surgeons using AI tools rather than autonomous AI systems.
How accurate is AI at predicting surgical outcomes?
AI accuracy varies by specific application. For predicting transfusion needs in knee arthroplasty, machine learning algorithms achieve AUC values up to 0.842. For implant sizing in knee replacement, AI models show femoral component accuracy ranging from 88.3% to 99.7% within one size deviation. For some preoperative planning tasks, accuracy exceeds 90%. However, accuracy for complex clinical decision-making remains limited.
What are the main barriers preventing AI from replacing surgeons?
The main barriers include technical limitations in handling anatomical variability and unexpected findings, lack of general intelligence for complex decision-making, inability to provide empathy and patient communication, underdeveloped regulatory frameworks, liability concerns, limited patient acceptance, and the fundamental challenge that surgery requires creative problem-solving and judgment that current AI cannot replicate. These aren’t merely temporary obstacles but represent fundamental gaps between current AI capabilities and requirements for autonomous surgery.
How will AI change surgical training and education?
Surgical training will evolve to include AI system operation, understanding of machine learning principles and limitations, skills in human-AI collaboration, and judgment about when to trust or override algorithmic recommendations. Trainees will need to master both traditional surgical techniques (for situations requiring manual intervention) and AI-assisted approaches. The curriculum will balance technical AI literacy with the irreplaceable human skills of clinical reasoning, communication, and ethical decision-making.
Conclusion: Enhancement Over Replacement
The question “Will AI replace surgeons?” implies a binary future that doesn’t match reality.
AI isn’t on track to replace surgeons—it’s transforming what surgeons do and how they do it. The technology excels at computational tasks: analyzing images, predicting risks, planning procedures, controlling precise instruments. It struggles with the fundamentally human elements of surgery: judgment, adaptation, empathy, ethical reasoning.
This isn’t a limitation waiting for better algorithms. It reflects the nature of surgery itself as a deeply human endeavor that combines technical skill with clinical wisdom, pattern recognition with creative problem-solving, and mechanical precision with compassionate care.
The surgeons of 2030 or 2040 will look quite different from those of 2020. They’ll work alongside sophisticated AI systems that handle routine tasks, flag potential problems, and augment human capabilities. But they’ll still be surgeons—making critical decisions, adapting to unexpected challenges, and caring for vulnerable patients in moments of crisis.
That’s not a failure of AI to reach its potential. It’s recognition that the most powerful applications of artificial intelligence in medicine amplify human expertise rather than replace it.
For patients, this means better outcomes through enhanced precision, improved safety through predictive analytics, and more time with surgeons who can focus on care rather than administrative tasks—all while retaining the irreplaceable benefits of human judgment, empathy, and advocacy.
The future of surgery isn’t surgeons versus AI. It’s surgeons and AI, working together to provide care that neither could deliver alone.
