Quick Summary: AI will not replace nurses but will transform how they work. The U.S. Bureau of Labor Statistics projects healthcare employment to grow through 2034, with AI handling administrative tasks like documentation and monitoring while nurses focus on complex patient care, clinical judgment, and the human connection that defines nursing. The profession requires adaptation, not replacement.
The question keeps healthcare workers up at night: will artificial intelligence make nursing obsolete?
It’s not paranoia. Technology replaces jobs constantly. But here’s what the actual data shows—and it might surprise anyone picturing robot nurses taking over hospitals.
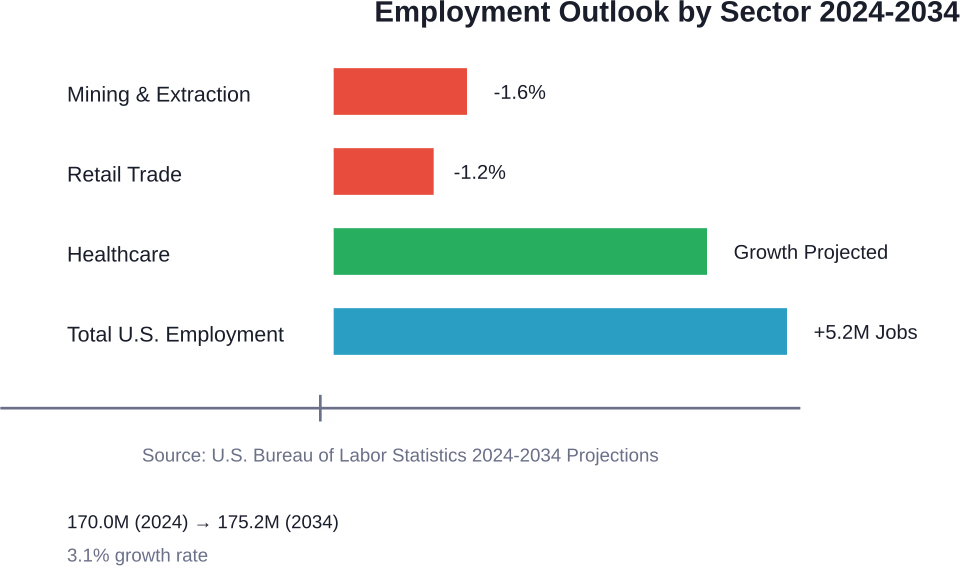
According to the U.S. Bureau of Labor Statistics, total employment is projected to grow from 170.0 million in 2024 to 175.2 million in 2034, an increase of 3.1 percent. Healthcare isn’t shrinking. And nursing? It remains one of the most secure career paths heading into the next decade.
Real talk: AI is already in hospitals. The question isn’t whether it’s coming—it’s what that actually means for nurses on the floor.
What the Employment Data Actually Shows
Numbers don’t lie, even when headlines do.
The Bureau of Labor Statistics released their 2024-2034 employment projections in August 2025. The U.S. economy is projected to add 5.2 million jobs over that decade. Healthcare remains a growth sector, not a contraction zone.
Now, some industries are declining. Mining, quarrying, and oil and gas extraction sectors are expected to drop 1.6 percent, driven partly by productivity gains through robotics and drones. Retail trade faces a 1.2 percent decline.
But healthcare? Different story entirely.
The projections don’t show nursing being automated away. They show evolution, not elimination. That’s a critical distinction that fear-mongering articles often miss.
How AI Currently Functions in Healthcare Settings
Let’s get specific about what AI actually does in hospitals right now.
Documentation eats up nursing time. Studies have shown that most nurses spend between 25-40% of their time updating patient information and electronic health records, including medication dispensation, vital signs, and care plans.
That’s where AI makes its biggest immediate impact.
Natural language processing can transcribe verbal notes. Automated systems pull vitals directly into electronic health records. Pattern recognition flags medication conflicts before administration. These aren’t futuristic concepts—they’re operational in 2026.
A 2024 survey reports that 66% of American physicians sampled use some form of AI in their practice. Nursing adoption follows similar trajectories, particularly for routine monitoring and administrative workflows.
But here’s what AI doesn’t do: hold a scared patient’s hand. Recognize subtle clinical deterioration that doesn’t show up in algorithms yet. Make complex judgment calls when protocols conflict. Navigate family dynamics during end-of-life discussions.
The Documentation Revolution
Data entry represents AI’s most mature healthcare application.
Voice-to-text systems convert bedside observations into structured notes. Computer vision reads monitoring equipment and auto-populates charts. Integration platforms sync data across hospital systems without manual entry.
Dr. Mehmet Oz, confirmed as the Administrator for the Centers for Medicare and Medicaid Services (CMS) in April 2025, stated he believes AI can “liberate doctors and nurses from all the paperwork.”
That’s the promise. Whether it delivers depends on implementation quality and system integration—areas where healthcare technology famously struggles.
Monitoring and Alerts
AI excels at watching trends across multiple patients simultaneously.
Continuous monitoring systems track vital signs and trigger alerts when parameters shift outside normal ranges. Sepsis prediction algorithms analyze multiple data points to flag early deterioration. Fall risk assessments update dynamically based on mobility and medication changes.
The challenge? False alarms. AI monitoring generates alerts that human nurses must verify, and high false-positive rates create alert fatigue rather than reducing workload.
Technology can assist, but it can’t replace the clinical judgment that distinguishes true emergencies from algorithmic noise.
Why Nursing Resists Full Automation
Some jobs automate cleanly. Assembly line work. Data processing. Routine calculations.
Nursing doesn’t fit that pattern.
According to research published in Nursing Management (2019), nursing fundamentally involves human connection, empathy, and complex decision-making that current AI cannot replicate. A position paper in Nursing Open emphasized that while AI can support nursing practice, the profession’s core requires human capabilities.
Community discussions among nurses consistently highlight what gets lost in automation conversations: the therapeutic relationship itself has clinical value.
The Empathy Gap
Patient outcomes improve when they feel heard and understood. That’s not touchy-feely sentiment—it’s measurable.
Compliance rates increase when patients trust their nurses. Pain management works better with psychological support alongside medication. Anxiety decreases when someone explains what’s happening in human terms.
In Korea, the Telemedicine Industry Council conducted a survey among 1,506 patients, 113 doctors, and 161 pharmacists who experienced non-face-to-face treatments, showing 93.2% patient satisfaction. But satisfaction with remote consultation doesn’t equal acceptance of AI replacement for in-person nursing care.
The difference matters.
Clinical Judgment Under Uncertainty
Textbook cases are rare. Real patients present with multiple conditions, conflicting symptoms, and situations not covered in standard protocols.
Experienced nurses develop pattern recognition that goes beyond algorithmic decision trees. They notice when something feels off before measurable parameters change. They adapt care plans based on subtle social cues and family dynamics.
AI operates on data it can measure. Nursing often operates on data it can sense.

The Push and Pull of AI Integration
Not everyone welcomes automation with open arms.
National Nurses United and other professional organizations have pushed back against certain AI implementations. The concerns center on patient safety, deskilling of the profession, and corporate cost-cutting disguised as innovation.
When Hippocratic AI initially promoted a rate of $9 an hour for its AI assistants compared with about $40 an hour for a registered nurse, concerns were raised throughout the profession. That’s not automation to improve care—that’s automation to cut labor costs.
The distinction matters enormously.
Real Implementation Challenges
AI in healthcare sounds great in PowerPoint presentations. Implementation tells a different story.
Systems don’t integrate smoothly. Electronic health records from different vendors don’t communicate. AI tools require clean data, but hospital data is messy. Training takes time nurses don’t have during understaffed shifts.
Research from the Journal of Medical Internet Research examining AI in critical care settings found that while AI can potentially alleviate healthcare shortages, successful implementation requires careful attention to workflow integration and staff concerns.
Technology deployed badly creates more work, not less.
The False Alarm Problem
Here’s what sounds good: AI monitoring every patient continuously, alerting nurses the instant something goes wrong.
Here’s what actually happens: AI generates alerts constantly. Most are false positives. Nurses spend time investigating alarms that don’t represent actual problems. True emergencies get lost in the noise.
Alert fatigue is a documented phenomenon. Adding more automated alerts without improving specificity makes the problem worse, not better.
Quality matters more than quantity when it comes to clinical decision support.

Focus On What AI Can Support In Care, Not Replace
AI is sometimes positioned as a replacement for nurses, but in real settings it works differently. It helps with structured tasks like data handling, monitoring, and documentation, while patient care, coordination, and real-time decisions still depend on people. AI Superior works with organizations that want to apply AI in a controlled, practical way.
They help define where AI fits inside existing workflows, then build custom solutions around those areas, combining consulting with development and integration so the tools actually work in day-to-day operations. If you are looking at AI in healthcare, it makes more sense to test it on specific tasks first.
👉Reach out to AI Superior to discuss your case and see what can be automated without disrupting how care is delivered.
How Nursing Education Is Adapting
Smart nursing programs aren’t pretending AI doesn’t exist. They’re teaching nurses how to work alongside it.
A framework published in Digital Health (2025) presents an argument that the profession should aim for ‘every nurse an AI nurse’—meaning AI literacy becomes a core competency, not a specialty.
That makes sense. Nurses who understand AI capabilities and limitations make better decisions about when to trust algorithmic recommendations and when to override them.
The American Nurses Association’s 2025 Code of Ethics addresses technology integration explicitly, with Provision 7.5 covering ‘Considerations Related to Ethics, Technology, and Policy’, recognizing that nursing practice now requires understanding how technologies from genomics to machine learning affect patient care.
| Skill Area | Traditional Nursing Education | AI-Enhanced Curriculum |
|---|---|---|
| Documentation | Manual charting, EHR basics | Voice systems, AI transcription, data verification |
| Clinical Decision Support | Reference texts, protocols | Algorithm interpretation, override judgment |
| Patient Monitoring | Manual vital checks, visual assessment | Continuous monitoring systems, alert management |
| Research Skills | Literature review, evidence evaluation | AI-assisted research, data analytics literacy |
| Communication | Patient interaction, team coordination | Plus telehealth platforms, AI interface design input |
What 2026 and Beyond Actually Looks Like
Predictions are cheap. Let’s focus on observable trends.
AI handles more administrative burden. Documentation becomes faster. Routine monitoring requires less manual effort. Scheduling and supply chain management get smarter.
But patient ratios don’t improve automatically just because technology exists. Hospitals still need humans at bedsides. Complex patients still need experienced nurses making judgment calls.
According to research published in Nursing Management (2019), global AI healthcare spending was predicted to equal $36.1 billion by 2025. That investment flows into tools that augment nursing work, not replace nurses entirely.
The nursing shortage remains real. Technology might help stretch existing capacity, but it doesn’t eliminate the need for human nurses.
Roles That Will Transform
Some nursing specialties will see bigger changes than others.
Remote patient monitoring expands as AI handles routine check-ins and escalates concerning trends to human nurses. Informatics nurses who bridge clinical practice and technology systems become more valuable. Nurses who can train AI systems on clinical workflows create new career paths.
But bedside acute care? Emergency departments? Critical care units? Those still need humans who can respond to rapidly changing situations with incomplete information.
The Productivity Question
Research published in the Journal of Nursing Management examining AI’s role in optimizing nursing productivity found that technology integration, AI utilization, and nursing competencies all affect outcomes—but leadership matters most for successful implementation.
Technology alone doesn’t boost productivity. How it’s deployed, who controls the implementation, and whether it actually addresses real workflow problems determines whether AI helps or hinders.
Nurses using AI tools helped design report better experiences than nurses having AI imposed on them by administrators who’ve never worked a floor shift.
FAQ About AI and Nursing Careers
Will AI completely replace nurses in hospitals?
No. AI will handle specific tasks like documentation and routine monitoring, but nursing requires complex human judgment, empathy, and adaptability that current technology cannot replicate. The Bureau of Labor Statistics projects overall employment growth through 2034, not nursing job elimination.
Should nursing students worry about job security?
Nursing remains one of the most stable career paths. The healthcare sector continues growing, and the nursing shortage persists. Students should focus on developing AI literacy alongside clinical skills—understanding how to work with technology rather than competing against it.
What nursing tasks will AI take over first?
Administrative work faces the most immediate automation: documentation, data entry, routine scheduling, and basic monitoring alerts. Tasks requiring physical presence, emotional intelligence, and complex decision-making remain firmly in human territory.
How much do AI nursing assistants cost compared to human nurses?
Some AI companies initially promoted rates around $9 per hour compared to approximately $40 per hour for registered nurses. But these systems supplement rather than replace nurses, and implementation costs, training time, and integration challenges add hidden expenses beyond the base technology price.
Do nurses need to learn AI programming?
Most nurses don’t need programming skills, but AI literacy matters. Understanding how algorithms make decisions, recognizing their limitations, and knowing when to override automated recommendations becomes part of core nursing competency. Informatics specialties may require deeper technical knowledge.
What’s the biggest risk of AI in nursing?
The primary risks involve poorly implemented systems that increase workload rather than reducing it, alert fatigue from excessive false alarms, and corporate cost-cutting that reduces nursing staff based on overly optimistic automation assumptions. Patient safety suffers when AI replaces nurses rather than assisting them.
Will telemedicine and AI reduce demand for hospital nurses?
Telemedicine shifts some care delivery methods but doesn’t eliminate the need for bedside nurses. Acute care, emergency situations, complex patients, and hands-on procedures still require in-person nursing. Remote monitoring may create new nursing roles rather than eliminating existing ones.
The Bottom Line on Nursing’s Future
Technology transforms professions without destroying them. Nursing in 2026 looks different than nursing in 2006, and it’ll look different again in 2036.
AI handles tasks that computers do well: processing data, recognizing patterns, automating repetitive workflows. Nurses handle what humans do well: connecting with patients, making judgment calls under uncertainty, adapting to unique situations.
The profession evolves. Nurses who develop technology literacy alongside clinical skills position themselves best for that evolution.
But replacement? The data doesn’t support it. Government employment projections show growth. Research emphasizes augmentation over automation. Even AI developers acknowledge that their systems assist nurses rather than replacing them—though implementation sometimes tells a different story than marketing materials.
So will AI replace nurses? No.
Will AI change what nursing looks like? Absolutely. And nurses who engage with that change—who help shape how technology integrates into patient care rather than having it imposed on them—will define what healthcare becomes.
The question isn’t whether to enter nursing given AI development. The question is what kind of nurse the profession needs as technology advances. One who understands both the science of care and the tools that support it.
That nurse? Still very much human.
